Fatigue, insomnia, depression, anxiety, low libido, poor stress tolerance, dry skin, poor quality sleep, apathy, sugar and salt cravings, repeated infections, headaches, slow wound healing, menstrual irregularities, diarrhea, constipation, hair loss, palpitations, cold hands and feet, poor body temperature regulation, low blood sugar, increased effort to perform daily tasks, lack of energy, food intolerances, allergies, etc...Chiropractor and naturopath Dr James Wilson, building upon the previous work of pioneers in the field of stress physiology, including Hans Selye, claims to have coined the term "adrenal fatigue" in 1998. Since then, a whole host of books have been published on the topic, and a simple google search brings up more than 403,000 results.
A brief introduction to "Adrenal Fatigue"
According to Wilson, the condition is roughly something like this:
Adrenal fatigue is a group of related signs and symptoms (a syndrome) that results when the adrenal glands function below the necessary level. Most commonly associated with intense or prolonged stress, it can also arise during or after acute or chronic infections, especially respiratory infections such as influenza, bronchitis or pneumonia.The adrenal glands are small glands situated on top of the kidneys, and are responsible for the production and release of a variety of steroid hormones, including cortisol, adrenaline (epinephrine) and, to some extent, noradrenaline (norephinephrine). These hormones are involved in a wide variety of regulatory processes like blood glucose control, regulating inflammation, energy mobilisation and metabolism, and the stress/fight-or-flight response (among other things - too many to list here), and without them we would be dead.
Adrenal fatigue is produced when your adrenal glands cannot adequately meet the demands of stress.*
During adrenal fatigue your adrenal glands function, but not well enough to maintain optimal homeostasis because their output of regulatory hormones has been diminished - usually by over-stimulation.* Over-stimulation of your adrenals can be caused either by a very intense single stress, or by chronic or repeated stresses that have a cumulative effect.*
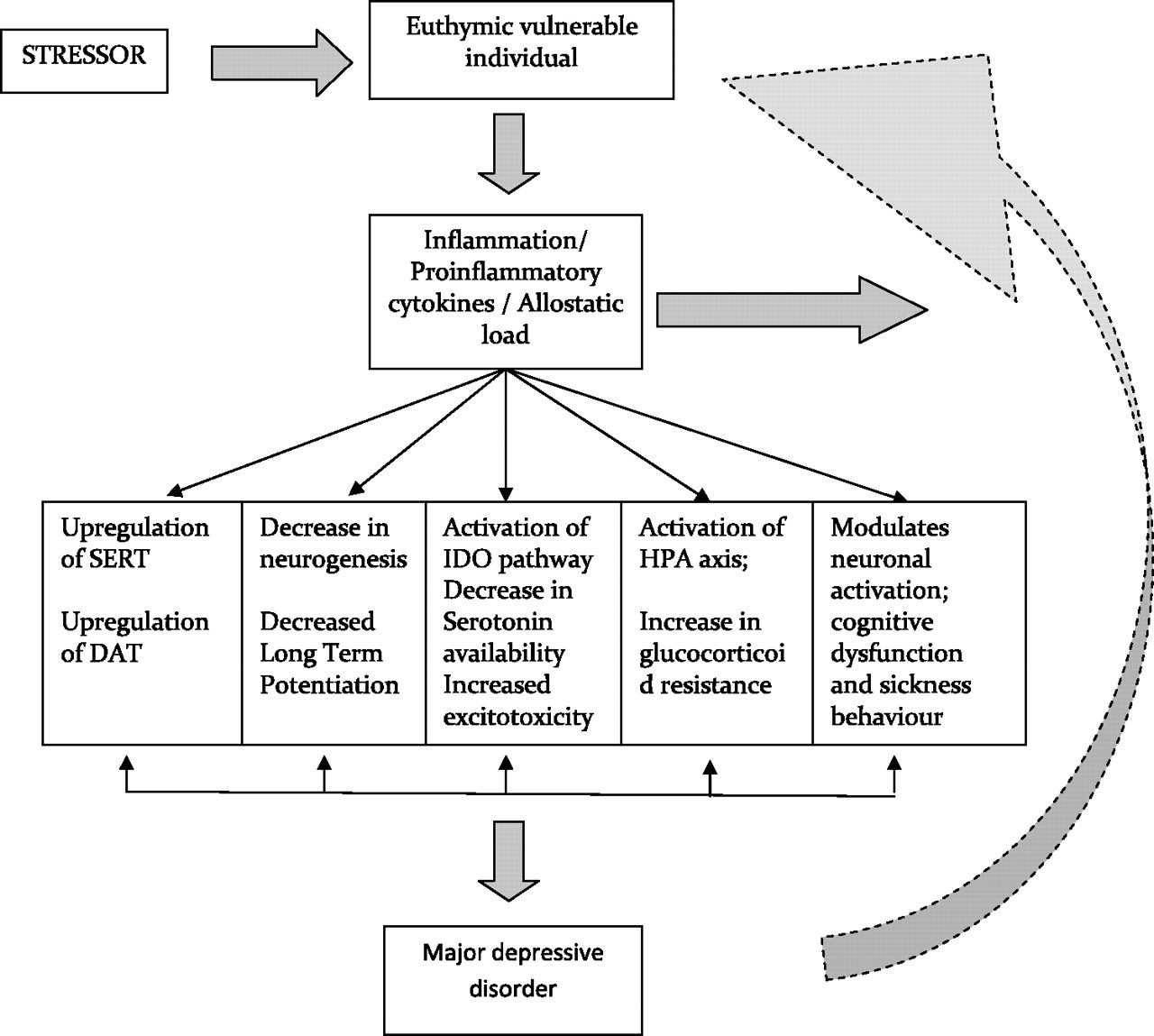
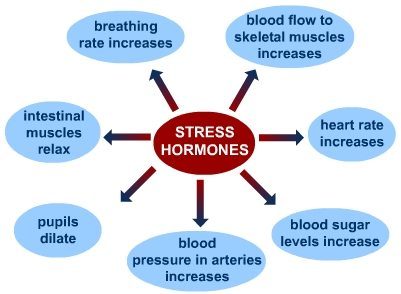
People often equate stress with psychologically or emotionally challenging events, such as the loss of a loved one, or pressure experienced at home or in the workplace. However, stress also takes place at the physiological level and it can be subtle enough to bypass conscious awareness. A stressor is any event or influence which disrupts balance or homeostasis. When the body encounters a stressor, it initiates a cascade of events referred to as the 'stress response'. The stress response involves a variety of physiological changes which are coordinated by the hypothalamic-pituitary-adrenal (HPA) axis and mediated primarily by stress hormones, including cortisol and adrenaline, and is designed to facilitate adaptation to adverse conditions by restoring balance within the system.
The hormone cortisol is secreted by the adrenal glands and begins to circulate in the blood. One of cortisol's main roles is to mobilise available energetic reserves (glucose) to be used for extra energy in the face of a perceived threat or lack of available resources. This makes it a catabolic hormone, meaning that it breaks down tissues, and can be particularly destructive to brain matter when left unopposed. As a counteractive measure, a hormone called Dehydroepiandrosterone (DHEA) is also released by the adrenal glands, and acts to protect against some of cortisol's destructive effects. Both of these hormones are naturally released in a 24-hour rhythmic fashion which is governed by the circadian rhythm and, under healthy conditions, the stress response should elicit the secretion of cortisol in the right proportion to DHEA.
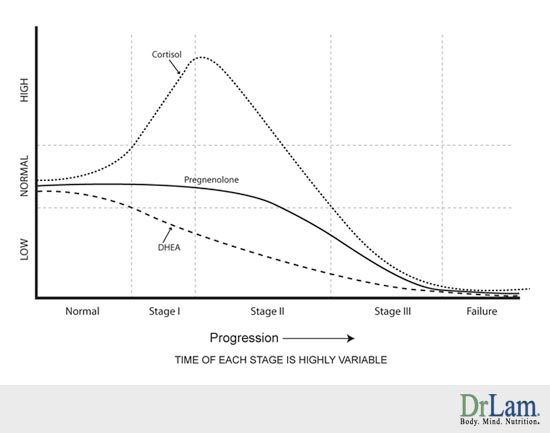
Popular models of adrenal fatigue state that its progression occurs in several stages. Initially, exposure to chronic or intense periods of stress can induce a state of "hyperactivity", characterised by persistently high levels of cortisol to meet the demands of the environment. This appears to skew the balance of these hormones towards a higher cortisol-to-DHEA ratio.
Pregnenolone steal: one (outdated) theory
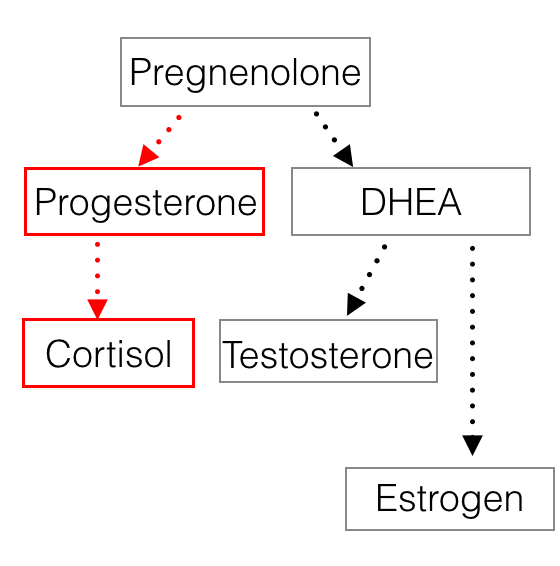
Since both cortisol and DHEA are derived from the same precursor building-block hormone pregnenolone, it is believed (through a process called "pregnenolone steal") that the finite pool of pregnenelone is used to produce cortisol at the expense of DHEA and other sex hormones further down the conversion pathway (estrogen and testosterone). In other words, pregnenolone is the raw material needed to make all hormones, so an excessive need for cortisol depletes the raw material, and therefore less can be used to build other hormones. The result = lower sex hormone production, high cortisol and low DHEA on a salivary hormone test.
Denial by conventional medicine: throwing the baby out with the bathwater
Despite an abundance of anecdotal evidence and clinical experience in alternative healthcare, the theory of "adrenal fatigue" has been called into question and criticised by many experts in the field of endocrinology and conventional medicine. One fairly recent systematic review published in BMC Endocrine Disorders concluded:
This systematic review proves that there is no substantiation that "adrenal fatigue" is an actual medical condition. Therefore, adrenal fatigue is still a myth.While there are a group of established medical conditions where adrenal output is severely compromised, such as in Addisons disease, adrenal atrophy, or in secondary adrenal insufficiency, there is no evidence that the adrenal glands fail to work in someone who does not have one of the above conditions. In fact, the adrenal glands actually appear to adapt very well to persistently stressful conditions, as can be evidenced by the fact that they increase significantly in size in response to chronic stressors. So from the perspective of conventional endocrinology, adrenal fatigue simply does not exist. And, in this case, mainstream medicine is actually partially correct.
But how can we reconcile this fact with the wide range of symptoms which thousands of people experience but who do not fall within the diagnostic criteria of Addison's disease or any other adrenal-related medical condition?
Well, a condition currently known as adrenal fatigue does exist, but the biology underpinning it was simply misunderstood. Although the premise that the "adrenal glands fail to work" may be physiologically incorrect, the experiences of people suffering from these symptoms should not be ignored and dismissed by conventional physicians. It is important to understand that terms like "adrenal fatigue", "adrenal exhaustion" and "adrenal burnout" have been used in the past to define and explain complex dysfunctional patterns related to the stress response. It is now understood that this dysfunction primarily originates from within the brain.
A brain-based disorder of HPA-axis dysregulation: Adrenal Fatigue is literally all in your head!
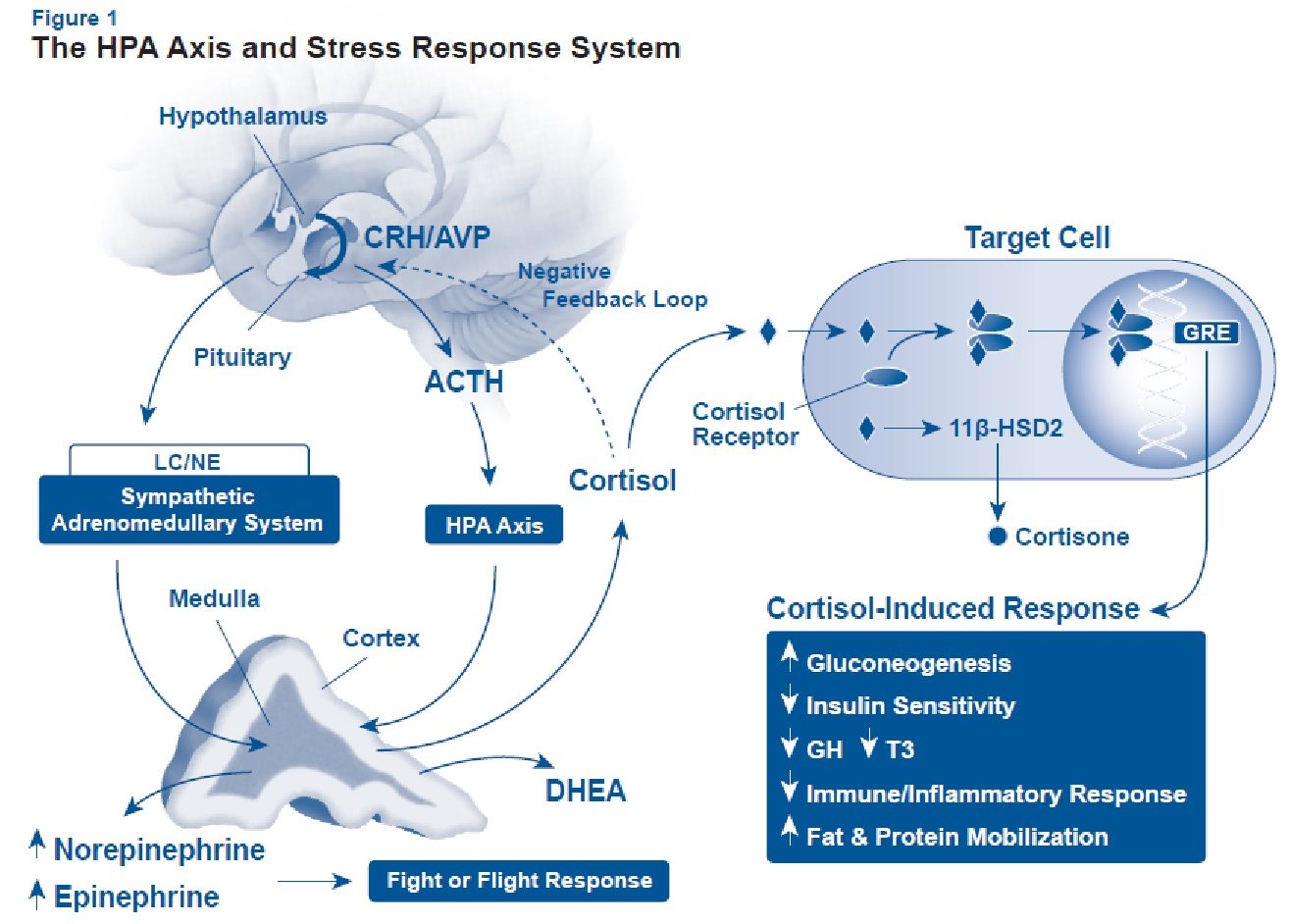
The brain is the central control system and the adrenal glands simply follow orders. The author of a paper titled "Physiology and neurobiology of stress and adaptation: central role of the brain" states:
The brain is the key organ of the response to stress because it determines what is threatening and, therefore, potentially stressful, as well as the physiological and behavioural responses which can be either adaptive or damaging.Rather than a failure of the adrenal glands to keep up with demand, the adaptive changes in stress-induced hormonal disruption are most often initiated within the hypothalamus and pituitary glands. The regulatory system governing adrenal stress hormone output (the brain) coordinates changes in response to internal/external informational inputs as an adaptation in adverse conditions. The stress response allocates metabolic resources and alters physiology to promote the short-term survival of the organism - often at the expense of long-term health.
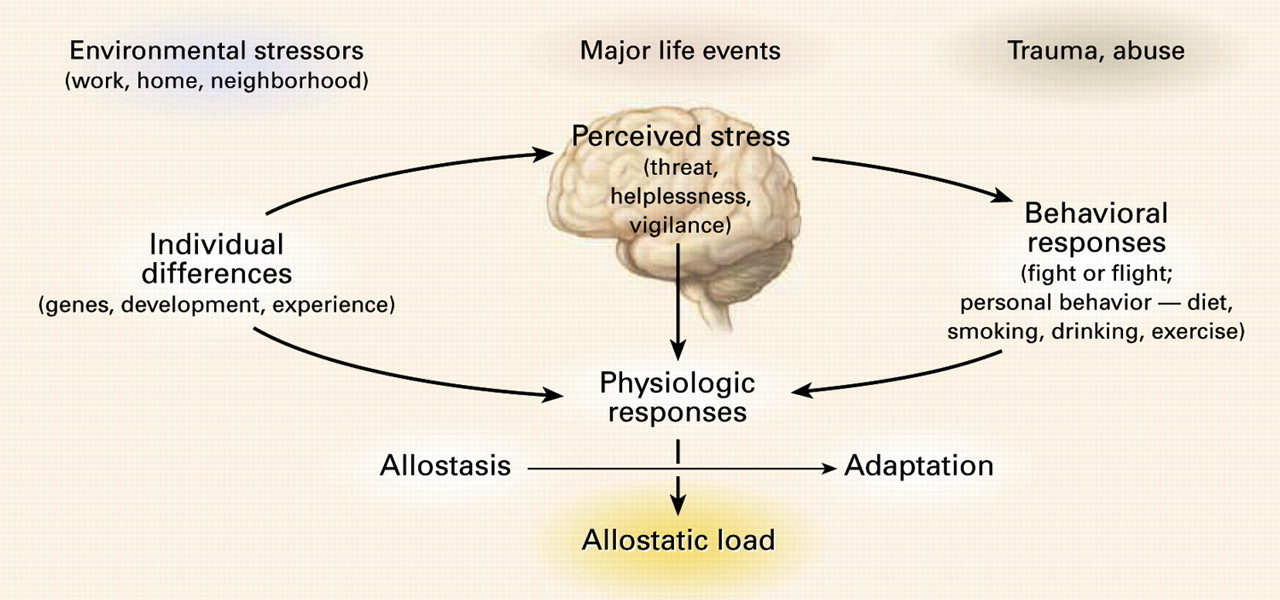
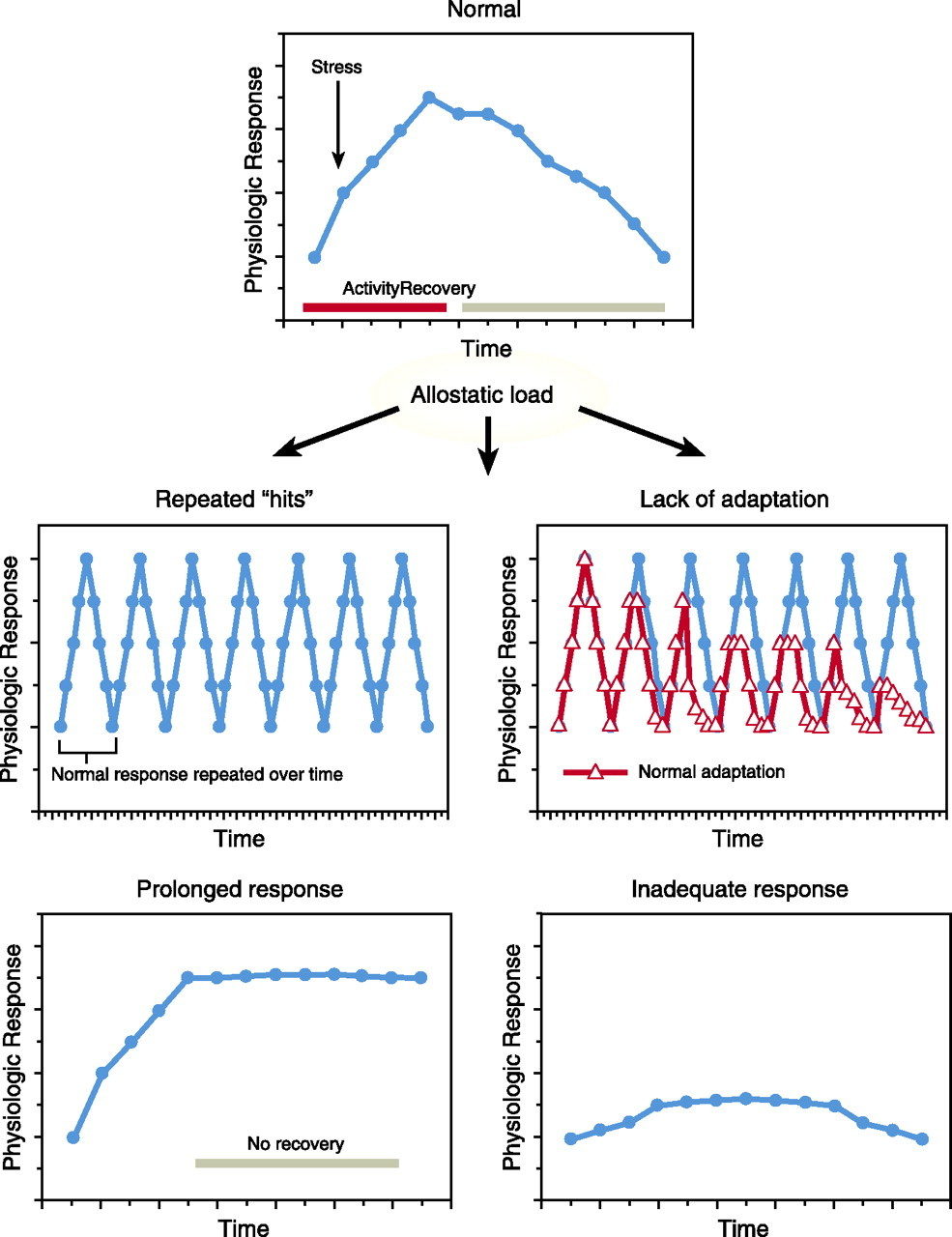
Why might this be? First of all, cortisol breaks down tissues including lean muscle mass, various organs and brain structures, particularly the hippocampus. Secondly, cortisol is a potent immunosuppressant, capable of suppressing immune cell function and ultimately lowering host immunity. Long-term exposure to high cortisol is enough to completely break down the system's defences and destroy entire organs. Therefore, to protect the body from infection and excessive tissue breakdown, it is possible the brain decides to reduce total hormone output and effectively "shut the blinders" until conditions improve. Unfortunately for many people, conditions do not improve, and so the long-term hazardous effects of low cortisol may begin to manifest.
Dispelling the myth of "Pregnenelone Steal"
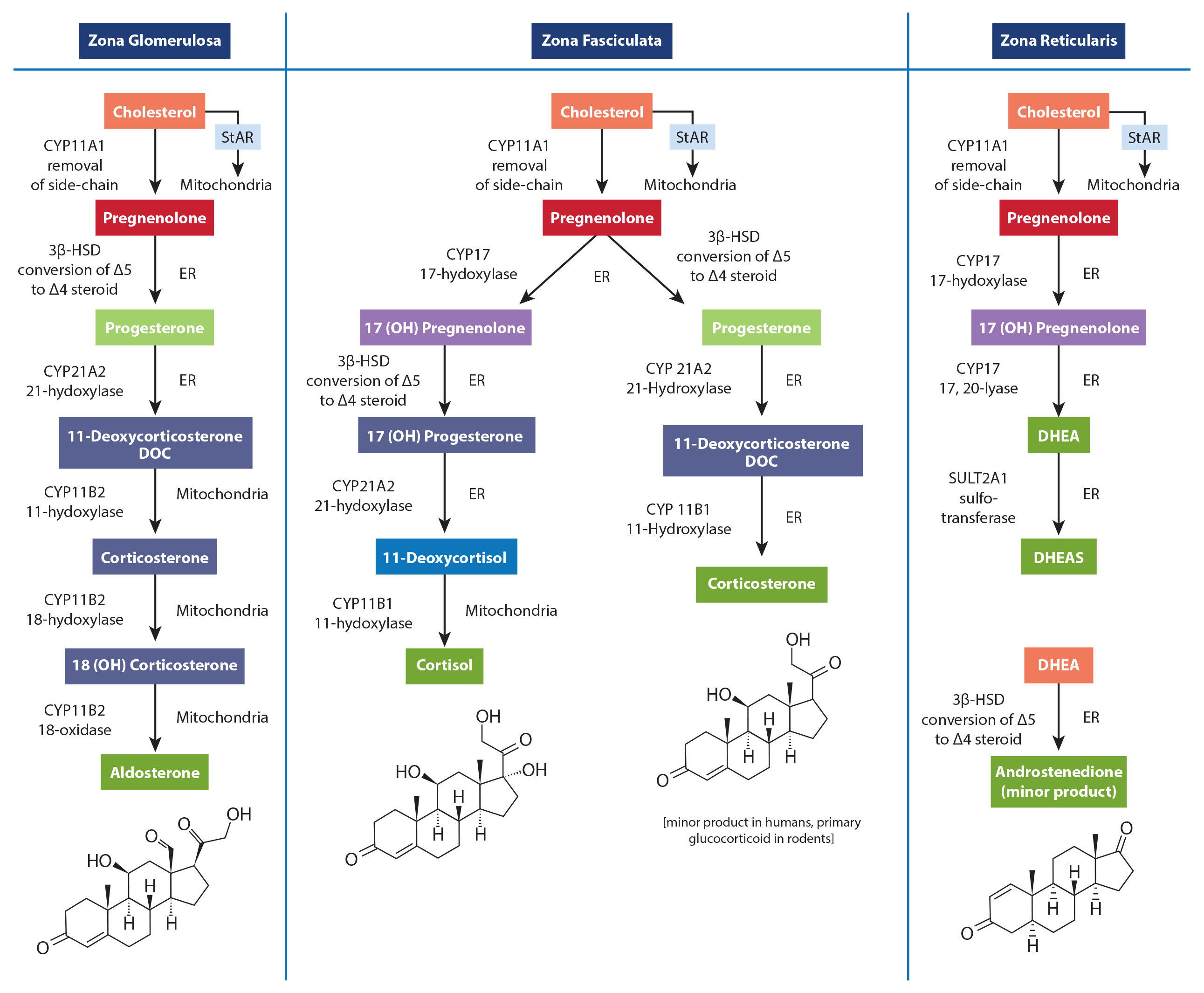
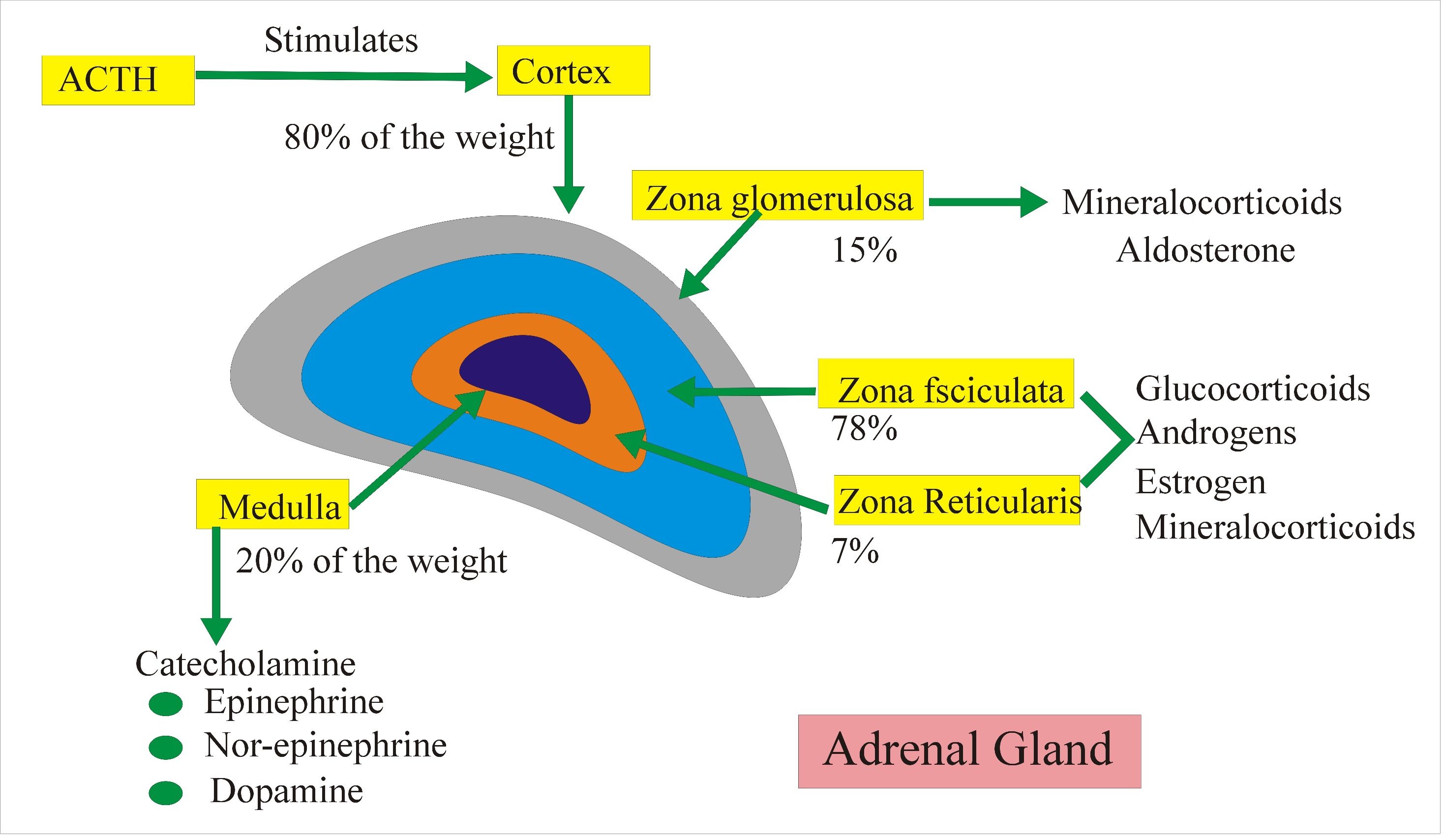
As shown in the diagram below, hormone production occurs in different tissues of the adrenal glands, and each tissue has its own unique types of cells. Recall what I wrote about pregnenelone being the building block of all steroid hormones. Well, that's not technically true. Cholesterol is actually the most basic raw material, which is converted into pregnenolone in the mitochondria of each respective cell, and then REMAINS in that cell.
Therefore, the notion that steroid hormone production uses pregnenolone from a single adrenal "pool" is fundamentally flawed. There is no known pool of pregnenolone that can transfer between the mitochondria of different cell types. Pregnenolone steal does not exist.
"...In addition, the ACTH-driven adrenal synthesis of cortisol is orders of magnitude higher than that of DHEA(S), and fluctuates radically within a 24-hour period. If there were an adrenal "pregnenolone pool" that contained enough pregnenolone precursors for elevated cortisol production in the morning (or during stress), this "pool" would then also be available for the much smaller amount of needed DHEA(S) production when cortisol synthesis drops even a little. Finally, as decades of steroidogenesis research has shown, the control of adrenal hormone output is regulated mostly by cell-specific enzyme concentrations and external signals coming from outside the adrenal gland.The four primary factors influencing HPA-axis dysfunction
[..]
While HPA axis stress and subsequent cortisol synthesis and secretion may coincide with the acceleration of reduced DHEA(S) production (i.e., a stress-induced down-regulation of DHEA(S)), this relationship is facilitated by regulatory processes (e.g., feedback inhibitions, receptor signaling, genomic regulation of enzymes, etc.), not an intra-adrenal depletion of pregnenolone as a precursor to downstream hormones.
In one study of poorly-controlled type 2 diabetic subjects with elevated cortisol and low DHEA levels, the enzyme necessary for DHEA formation in the zona reticularis (17,20 lyase) was shown to limit the production of DHEA. The enzyme activity was corrected (along with near normalization of cortisol, DHEA and DHEA-S levels) after six months of diet or pharmacotherapy to improve blood glucose control.26
Additionally, cell-culture studies suggest that under inflammatory stress (IL-4 and other cytokines), the zona reticularis will down-regulate DHEA production when ACTH is present.27,28 These and many other factors (e.g., aging) are likely the driving influenced affecting the dynamic relationship between cortisol (activated by the HPA axis) and measured DHEA and/or DHEA-S levels."
Circadian Disruption
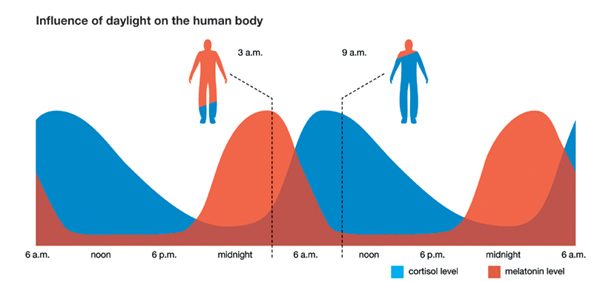
Sleep disturbances and a poor circadian rhythm acts as a powerful stressor and is independently capable of disrupting the HPA-axis. The HPA axis is directly tied to the circadian rhythm, with cortisol typically following a 24-hour cycle that can been seen in the graph below.
Here is an excerpt from one paper on the topic:
Evidence suggests that various hormones and metabolic processes are affected by sleep quality and circadian rhythms; such interactions are mediated by numerous clock genes. Hormones such as growth hormone, melatonin, cortisol, leptin, and ghrelin are closely associated with sleep and circadian rhythmicity, and endogenous circadian-regulating mechanisms play an important role in glucose and lipid homeostasis. Sleep disturbances and, particularly, deprivation are associated with an increased risk of obesity, diabetes and insulin insensitivity, and dysregulation of leptin and ghrelin, which negatively impact human health. Circadian disruption, which is typically induced by shift work, may negatively affect health due to impaired glucose and lipid homeostasis, reversed melatonin and cortisol rhythms, dysregulation of leptin and ghrelin, more severe metabolic syndrome, and clock gene rhythm loss.For more information, I have written about the effects of artificial light at night and the importance of maintaining a circadian rhythm in this article.
Glycemic Dysregulation
Cortisol's technical classification is a "glucocorticoid", and this reflects cortisol's role maintaining blood glucose concentrations. When the blood sugar swings low (like in a stressed state), the body relies on cortisol to shred muscle tissue and activate glucose production in the liver. This provides energy for short-term use, but can be severely detrimental when it occurs long-term.
People with poor blood glucose control (insulin resistance, eating foods which spike blood sugar excessively) may experience a "crash" (drop in blood sugar) shortly after eating a meal and induce a cortisol response. Meal timing is also important, since it has been shown that meals in the evening evoke a larger spike in blood sugar than those eaten earlier on in the day and subsequently increase the likelihood of cortisol secretion. Hence, effectively managing blood glucose with dietary interventions and lifestyle changes should theoretically help in this regard.
Inflammation
Pro-inflammatory cytokines such as interleukins 1, 6 and TNF-alpha act directly on the hypothalamus to increase the production of cortisol. Cortisol is a potent anti-inflammatory agent and is signalled when there is either acute or chronic inflammation somewhere throughout the body. Chronic low-grade inflammation may go unnoticed, yet contribute significantly to the overall allostatic load. Low-grade inflammation may be coming from hidden food intolerances, undiagnosed allergies, leaky gut, chronic inflammatory conditions & autoimmune processes, central adiposity/obesity, mould exposure, chemical toxicity, heavy metal exposure, or anything else which the body deems to be a threat.
It has been proposed that long-term exposure to proinflammatory cytokines can induce a state of "cortisol resistance", whereby glucocorticoid receptors become less sensitive and so cortisol cannot exert its anti-inflammatory action of cells. The dynamic interplay between immune cells and the HPA axis is bi-directional, which means that there is a two-way street of communication. Chronic inflammation can cause HPA-axis dysregulation and excessive stress hormones, whereas prolonged exposure to stress hormones can also lead to chronic inflammation.
Emotions associated with stress such as grief, fear, guilt, anxiety, excitement, and embarrassment all trigger a response from the HPA-axis and increase cortisol. Events such as public speaking or a trip to the dentist's office also elicit similar physiological responses. However, the severity of the response and the ability to recover is highly individual and has more to do with a person's perception of the event, rather than the actual event itself.
According to Thomas Guilliams PhD:
The four key factors that determine the magnitude of the HPA axis response to a mental/emotional stressor are its 1) novelty to the individual, 2) unpredictable nature, 3) threat to their person or ego, 4) sense of loss of control. Individual characteristics of the patient are also profoundly influential. Innate qualities such as age, gender (female preponderance) and hereditary predisposition, coupled with personality characteristics (i.e. introversion and low self-esteem) and prenatal and early childhood experiences, serve to further individualize and amplify each patient's unique stress response.Here is why it is important to pinpoint those aspects of your life which you feel cause you the most stress, and then find ways to take appropriate precautions and hopefully bypass what is unnecessary. Of course, it is impossible to predict when stressful life events will take place, and some stress is just unavoidable. However, if we take the time to observe and be honest with ourselves, we can very quickly gather data and gain some insight into the various patterns of behaviour which surround subjective feelings of stress.
For example, you may notice that you become stressed out in the morning time because you are rushing to make it to work on time. In this case, you could make some simple changes like waking up half an hour earlier, or packing your lunch the night before. It is those basic changes that can truly make the world of difference when it comes to improving health.
Conclusion
The pathophysiology of "adrenal fatigue" is characterised by dysfunctional patterns related to the HPA-axis. Since there is no research to substantiate the idea of adrenal glands becoming fatigued or failing to work in any way, it is more appropriate to refer to the condition as HPA-axis dysfunction/dysregulation.
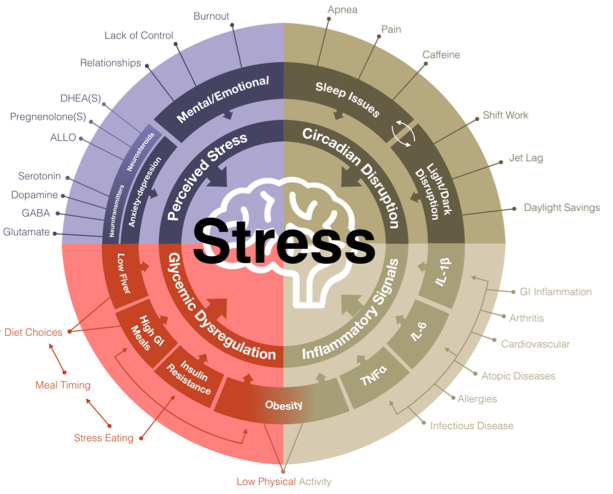
The exact causes of HPA-axis dysregulation appear to be complex and multifaceted. Research has provided evidence that four key areas are involved: 1. perceived stress, 2. blood sugar control, 3. circadian rhythms, and 4. inflammatory processes.
With this considered, the use of supplementation designed to "support the adrenals" may not be sufficient to aid in recovery unless the underlying causes of HPA-axis dysfunction have been identified and addressed.




Reader Comments
I would start by looking at the four main areas :
1. Blood sugar control - Is a person effectively managing their blood sugar, or is it like swings and roundabouts? Are they eating too often, or not enough? Does someone eat in a stressed out state, or do they practice mindful eating? Is the food whole foods, or refined junk? etc
2. Inflammation - Does this person suffer from some kind of inflammatory condition? Is there hidden inflammation coming from the gut, how is their digestion working, is detoxification working properly? Do they have a history of heavy metal exposure or chemical exposure? This stuff can be identified with some functional testing if you work with a practitioner.
3. Perceived stress - Is there unresolved trauma as in some form of PTSD? Does this person regularly exhibit behaviour which promotes stress? Does their daily routine involve stress? Simple, basic changes can be implemented to reduce this stuff, or maybe psychotherapy for those who have more severe issues.
4. Circadian Dysregulation - Does this person get half an hour to an hour of morning daylight each day? Are they blocking blue light at night time? How well do they sleep? Waking up groggy and tired, or full of energy? These are question I would ask to ascertain the quality of the circadian rhythm.
I am not sure about pressure points, but someone with more knowledge in this area may be able to chime in. As per my understanding, the brain makes adaptive changes to compensate for a stressful environment. So fixing the rhythms and hopefully changing the function of the brain (and associated systems) should hopefully occur naturally if someone hits all of the above bases.
Thank you so much for your instant response! I was eager for info for sure.
I have (and had for years) the fatigue alright but knew my adrenals were fine. Now you ve explained it to me!
I ve been very diligent with regards to all of the above except for the bluelight, which i have corrected however. (thanks HFL!) AND... life s challenging obstacle course, well, one has to hold on whilst riding the big mega mf waves O_O
Thank goodness thems have majorly calmed down!
Slow n Steady wins the race eh?