
© Alamy
The government is pledging to end smoking in England by 2030
as part of a range of measures to tackle the causes of preventable ill health.
Promoting physical activity, developing guidelines on sleep and targeting those at risk of diabetes are also set out as priorities in the green paper.
The policy document aims to reduce the number of years spent in poor health.Currently men and women spend over a fifth of their lives in ill health - 19 years for women and 16 for men.Those in deprived areas experience the longest periods of poor health.
The green paper, which will now be consulted on, proposes a number of ways of tackling this.
They include:
- Ensuring any smoker admitted to hospital automatically gets offered help to quit
- Extending tooth brushing schemes in nurseries and primary schools
- Reviewing the evidence on sleep and health with a view to developing clear national guidance on daily recommended hours of sleep
- Encouraging "active play" such as skipping in nurseries and more travel by bike and on foot
- Doubling funding for the diabetes prevention programme which targets lifestyle support to those most at risk of developing type 2 diabetes
The measures come on top of steps that have already been consulted on, including:
But the publication of
the green paper was immediately criticised after it was slipped out just ahead of the announcement of a new prime minister on Tuesday.Helen Donovan, of the Royal College of Nursing, said: "We've been waiting some time for
these plans which appear to have been buried in the dying days of the current government."She also warned that the plans "already start at a disadvantage" as
the money councils get to run healthy lifestyle programmes is being cut.Councillor Ian Hudspeth, of the Local Government Association, said the green paper contained some "ambitious and interesting ideas", but agreed it would be undermined by the inadequate funding.
Why publish now?The manner of the green paper's publication left most in the health world scratching their heads.
It was slipped out online late in the evening by the Cabinet Office and not the Department of Health and Social Care. There was no press notice.
It's understood Theresa May was determined to get it out in the last days of her premiership, while Health Secretary Matt Hancock wanted to delay it till the new administration was formed.
Front-runner Boris
Johnson has made it clear he is opposed to more sugar taxes and similar interventions.Mr Hancock is thought to have wanted to see how the new Prime Minister might approach the issues covered in the paper.
Shadow health secretary Jonathan Ashworth branded the green paper "extremely disappointing", highlighting the decision
not to push ahead with extending the sugar tax to milkshakes - the paper proposes waiting to see if industry reduces the sugar content of milk drinks.
There is no commitment either to introduce a levy on tobacco firms to pay for stop smoking services -
something which had been called for.
Previously the government had aimed to create a smoke-free society - with smoking rates close to zero - by 2025. Currently 14% of adults smoke.The consultation on the green paper runs until 14 October, with the government's response expected by next spring.
Comment: More from the BBC:
Who are the smokers that haven't quit?
In 1974, almost half of all adults in the UK smoked. For many, spending time in smoke-filled homes, pubs and workplaces was simply a part of daily life.
Today, that figure has fallen to 15%. The government has pledged to end smoking in England altogether by 2030.
But some people remain much more likely to smoke than others.
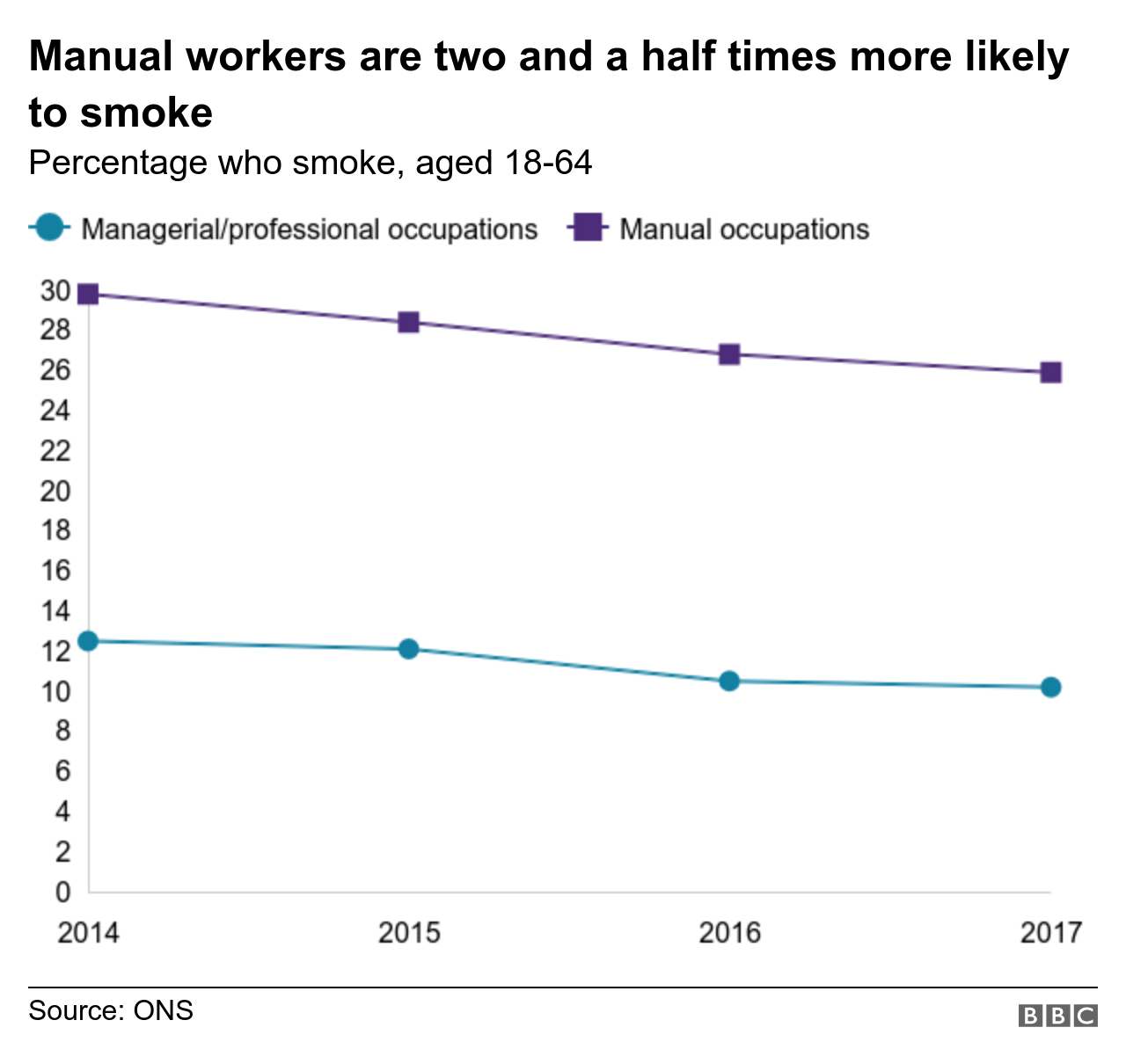
People living on a low income are disproportionately likely to smoke, for example. One in three social housing residents and one in four manual workers smokes, compared with one in 10 of those in professional or managerial jobs.
Smoking rates also differ considerably around the country. Only 8.6% of those in East Devon smoke, for example, compared with 21.8% in Dundee.
This regional divide is startlingly illustrated by the proportion of women who smoke while pregnant.
In England, one in 10 pregnant women smoke. But within this there are huge variations - ranging from one in 50 in some wealthy parts of London to one in four in Blackpool, one of the most deprived areas.
People with mental health problems are similarly affected. This group is 50% more likely to smoke than the rest of the population, a gap that has been widening.
Because smoking is so uniquely harmful, this translates into major differences in illness and early death.
One US study suggested smoking accounted for two-thirds of the life expectancy shortfall among people with mental health problems, 10 years of lost life. These findings are likely to apply to other countries too.
Another study indicated the poorest men in England and Wales were twice as likely to die between the ages of 35 and 69 as the richest - and their death was almost five times more likely to be caused by smoking.
Why are these groups more at risk?
In recent years, the UK has introduced policies that appear to have helped many smokers quit and deterred others from starting.
The smoking ban was introduced in 2007, alongside a raising of the minimum purchasing age to 18.
Taxes on a £10 pack of 20 cigarettes have increased to over 80% of the retail price, while the packaging and display of tobacco products have become increasingly restricted and advertising banned.
Wales is targeting a 16% smoking rate by 2020, while the Scottish government aims to create a "tobacco-free" generation by 2034 and Northern Ireland is also aiming to eradicate smoking altogether, in addition to England's pledge to end smoking by 2030.
Stop-smoking services providing support and medication have also been offered nationwide, contributing to the fall in overall smoking rates.
Yet they have been less effective for poorer and mentally ill smokers, even if they are as likely to try to quit as other groups.
The reasons for this are varied and complex.
These groups can have higher levels of dependence, making it harder to give up. They are also more likely to be around other smokers, normalising the behaviour and making it harder to quit successfully.
They may also have to deal with stress factors such as income instability, poor housing and living in run‐down neighbourhoods.
At the same time, stop-smoking services, which appear to have helped reduce inequalities, have disappeared in many areas, with an estimated 30% funding cut in England between 2014-15 and 2017-18 .
Financial incentives
For these reasons, a different approach may be needed.
Some clear recommendations have been made to stop the third of mentally ill people who smoke from being left behind. Many can be applied to other at-risk groups.
Free, tailored individual support, including advice, mobile stop-smoking services and online resources, has been shown to be effective, as have financial incentives such as making cigarettes more expensive and offering smokers cash to quit.
Price increases appear to work best in combination with support such as counselling and smoking alternatives such as electronic cigarettes or nicotine patches.
E-cigarettes, in particular, have become more popular in recent years. Public Health England suggests these products carry a fraction of smoking's risk and every year could be contributing to between 22,000 and 57,000 people quitting smoking.
Doctors asking patients if they smoke could also help identify would-be quitters who don't want to bother the NHS or are facing multiple health conditions.
Why is this so important?
Reducing smoking among the most disadvantaged is one of the most important ways to reduce health inequalities.
Alongside shortening life expectancy through disease and illness, smoking can also negatively affect mental health.
Giving up is associated with reduced depression, anxiety and stress, while boosting overall quality of life.
The addiction is often passed from one generation to the next, meaning children who grow up around smokers are much more likely to take it up themselves.
On top of this, smoking is expensive and can trap people into cycles of poverty.
While far fewer people smoke now than in the past, there are still seven million smokers in the UK.
Studies suggest most long-term smokers die from a smoking-related disease.
Every year in England, 80,000 people die from the effects of smoking, making it the number one risk factor for ill health and early death.
With more than 200 deaths per day, this is equivalent to a plane crashing every day.
About this piece
This analysis piece was commissioned by the BBC from an expert working for an outside organisation.
Dr Leonie Brose is a senior lecturer at the National Addiction Centre, King's College London.
It's bears repeating: Smoking rates have plummeted yet diseases and illnesses of all kinds are on the rise, and so, evidently, tobacco - with it's numerous, proven health benefits - is not to blame. While poverty continues to rise and quality of life deteriorates throughout the Western world, rather than coordinate a plan to alleviate the causes of this suffering,
governments are instead prioritising the banning of tobacco.
The anti-smoking agenda is nothing new and much of the theory and coercive techniques come thanks from the Nazi Germany. Those lauding the anti-smoking agenda should be careful what they wish for:
See:
Also check out SOTT radio's:
The Health & Wellness Show: The Truth about Tobacco and the Benefits of Nicotine




My best guess is that only by granting free will can God experience individuality, from singularity.
Singularity is what happens in the after-life, I think.