Running Time: 01:42:43
Download: MP3
Here's the transcript of the show:
Jonathan: Welcome to the Health and Wellness Show everybody! Today is Friday, April 22, 2016; my name is Jonathan and I'll be your host for today. Joining me in our virtual studio from all over the planet, and I mean from all over; people have been trading places across continents and it's crazy all the travel we have going on, but we have Doug, Erica, Tiffany and Elliot. Welcome guys!
All: Hellos
Jonathan: And we miss Gaby today, she can't be with us so we wish her well and hope that she is able to come and join us next week. Let's see, today our topic is inflammation and we're going to be talking about all the different types of inflammation. What are the causes, is it acute inflammation, is it chronic and what are the results of inflammation, because it's something that listeners of our show may be aware of; inflammation's role in disease, especially from reading the forum. There is a lot of talk that goes on there, but especially over the last number of years a lot of research on the forum has uncovered the fact that inflammation is essentially the root cause of most, if not all disease.
Of course there are causes of inflammation itself but inflammation is the theme that you want to treat when you are looking to alleviate many, many different conditions. We are going to talk about that today and hopefully shed some light on the topic and if anybody has not been familiar with this, hopefully it will turn on some lightbulbs for you and maybe give you a different approach to whatever might be going on and different ways that you can treat it.
Let's get started. I guess to kick off the discussion I wanted to talk a little bit about what inflammation is. I'm sure anybody who has a grasp of language understands the concept of what inflammation is but we can get a little bit into the details about what happens when your body is inflamed and how inflammation can actually be a positive. It's a thing that your body does as an indicator of something that is going wrong.
When we were talking before the show and planning the show, I know that Elliot, you had brought up the concept that inflammation can actually be a good thing, but I wondered if you wouldn't mind just riffing on that for a little bit and then we will get into the differences between chronic and acute inflammation; if that's ok?
Elliot: Inflammation, for those who aren't aware of the term inflammation or don't really understand what it actually is, inflammation is basically the body's response to an invader. It can be a pathogen; it may occur for instance when you cut your hand. What happens is straight away your body initiates a response in which your hand will start to swell up, the blood will clot and then it will start to form a scab. This is acute inflammation and is actually very important; it's your body's response to an outside agent and is the way in which the body acts to protect and heal where there is an injury or infection.
Tiffany: Inflammation is basically just redness, swelling, heat and pain. Like if you have an experience when you've sprained your ankle and you look down and you notice that it's swollen, you feel it and it feels a little warm and might turn a little red and of course it hurts, and then you can't walk on it so you use a little function; that's basically what inflammation is. It literally means "on fire" and like Elliot was saying, it's a response to any kind of invader like a pathogen or an injury or a toxin or a heavy metal, a virus or anything like that can cause an inflammatory response.
Doug: I think there is a big difference between the acute inflammation and chronic inflammation. An acute situation is when you get a splinter then all of a sudden it gets all red and puffy around where the splinter entered and that actually is a good thing because that's actually helping to fight off all the possible pathogens that might have got in with it and it's helping to repair the area. There is increased blood flow obviously, to get more of the immune factors there to help with that but the problem is that when you have a chronic inflammatory situation where your body is constantly mounting this inflammation response, that's when things can get really bad because your body is not designed to be in a constant state of inflammation.
If you look at something like say, gut inflammation from eating a toxic food of some kind, your gut should not be inflamed all the time. If you take that splinter example and imagine you got it in your knuckle, you can see how you would lose function in your knuckle, like you can't bend it as much as you usually would do. Imagine your gut trying to function like that all the time and you can start to get a picture of how bad that can be if that inflammatory response becomes a chronic situation.
Erica: Dr. Mark Hyman talks a lot about it and he wrote a book about an anti-inflammatory diet. He talked about how the list of causes of inflammation is relatively short. Like Doug was saying, poor diet, mostly sugar, refined flours, processed foods and trans fats. Stress is another one and hopefully we will get into how to deal with stress and inflammatory issues; hidden or chronic infections, viruses, bacteria, parasites and then also allergens from food and the environment; toxins like Tiffany mentioned, mercury, pesticides, heavy metals; also moulds.
Dr Mark Hyman has a pretty good little 100-page book about how to start recognising inflammatory foods and how to cut them out of your diet; also nightshades are also an inflammatory food.
Tiffany: Speaking of Mark Hyman, he also talked about fourteen signs of inflammation because a lot of people hear inflammation and they don't equate it to what's going on with themselves. He says you're:
- BloatedAnd interestingly enough, craving certain foods. Sometimes we will crave the very foods that we shouldn't be eating because it gives you that opioid kick and it helps the pain go away. So if you crave certain foods then you should think that maybe something is going on with some kind of inflammation process. He also says compulsive or binge eating should go along with that.
- Belch a lot
- Pass gas
- Diarrhoea or constipation
- Fatigue and sluggishness
- Itchy eyes or itchy ears
- Dark circles or bags under your eyes
- Joint pain and stiffness (like with arthritis)
- Irritated throat or tickly cough without being sick or having a cold
- Stuffy nose or sinus trouble
- Excessive mucus
- Acne
- Cysts
- Hives
- Rashes
- Inflamed looking skin
- Flushing on the skin
- Water retention and skin puffiness
Oddly enough he doesn't have headaches on there, I think that's a sign of inflammation too. Those are some of the signs that Mark Hyman lists that are signs of inflammation.
Jonathan: There is something interesting that I got from the Hyman article that is up on SOTT called Is your Body Burning Up with Hidden Inflammation? That is more of a chronic condition as opposed to the acute although it can be acute. Chronic inflammation is a little bit more on the hidden side of the spectrum I think and there is a quote from the article where he said "A study of a generally "healthy" elderly population found that those with the highest levels of C-reactive protein and interleukin 6 (two markers of systemic inflammation) were 260 percent more likely to die during the next four years." So that's quite an increase. The increase in deaths were due to cardiovascular and other causes but the hidden, systemic inflammation can really be damaging and it's something that you don't really notice unless you are paying attention to the signs that your body is kicking out or you are really watching your diet and what's going on.
Even in cases where you are watching your diet you might be in some sort of a transition phase where you are trying different things to see what works and what doesn't. I haven't done this test yet but some of us have recently discovered that they react to eggs and when I do the test I'm really hoping I don't because I love eggs. There are certain things where you might think that this is ok, this is part of the paleo/keto diet and then you might find out that your body just reacts to that with an inflammation response. Of course if you eat something like that on a regular basis then you can end up with chronic inflammation.
Erica: With the eggs, it might be the fact that, especially in the US, the chickens are so full of hormones and antibiotics. It would be interesting to do a little research if you had your own chickens that weren't pumped full of god-knows-what to see if you reacted to the eggs in the same way.
Jonathan: It's an interesting issue. I've known two people who were lactose intolerant who then tried raw milk and didn't have a response to it. They may have been reacting to the hormones and the antibiotics in processed dairy. That's a hard one to say.
Inflammation is one of the dry medical topics. I think there is a really fascinating side to this which is that idea that it can rage in your body unnoticed; even for years and years and you won't notice the effects until they build up and get really bad and then you are like "I have this condition now, where did it come from?" In many, many cases, it came from your diet over the course of many years or chronic stress from a job or from your state of mind. All of these things can contribute to a de-generation in health.
Tiffany: If you are at your doctor's office and they say you have arthritis or you have pericarditis or atherosclerosis, anything with "itis" or "osis" on the end of it, basically means that part of your body is inflamed. In my mind, if that one part of your body is inflamed then you can assume that other parts are inflamed too because they have to travel to that part of your body in order to get inflamed so there is probably inflammation on the way to that part. Basically anything with "itis" or "osis" on the end means inflammation.
Doug: It's too bad, somebody should be treating the inflammation but the mainstream medical community is so segmented and there isn't a holistic picture of what's going on. So what they will do is send you to a specialist for that particular organ and have you deal with that person, but really dealing with systemic inflammation is the same method overall which is to find out the cause and deal with that to decrease the inflammation, rather than send somebody to a specialist on a particular organ and have them come at it from a very closed perspective; just deal with the overall inflammation and then you will probably see a great deal of improvement.
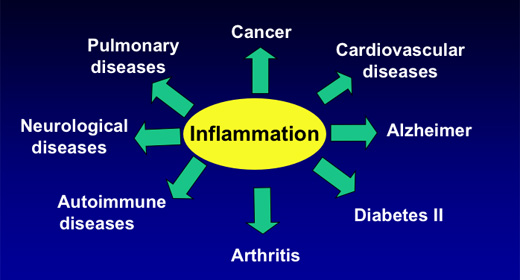
Erica: That's what Dr. Mark Hyman talks about in the article Jonathan mentioned. Inflammation run amok is at the root of all chronic disease, like heart disease, obesity, diabetes, dementia, depression, cancer and even autism. Going back to that gut connection that Doug mentioned, the dysregulation of the gut, they see that in a lot of autistic children and when they clean up their diet and they remove inflammatory foods, like gluten, these autistic children turn around in a lot of cases.
Doug: It's not really in mainstream circles at all but people are getting their autistic kids on these diets which remove a lot of the inflammatory foods from the diet and they are seeing big changes. It's essentially an anti-inflammatory diet, take out the gluten, take out the dairy, take out nightshades and any other classically inflammatory foods. That is even without getting any kind of testing to see which sorts of foods they might be reacting to individually; like Jonathan was mentioning, eggs.
They are not thought of as a common inflammatory food but a number of people do react to them. So there are different stages of getting rid of this inflammation, first you get rid of the stuff that is inflaming everybody, then you figure out what's inflaming you on top of that.
Jonathan: If I remember correctly, there was even some discovery on the forum about coconut; coconut oil and coconut milk; that certain people reacted to that in a negative way.
Tiffany: Coconut oil is promoted as one of the really great oils but not everybody can tolerate it. That's why it is so important to find out what bothers you specifically, even though other people may be able to eat it without experiencing any problems what-so-ever.
Doug: It's funny because I'll try to avoid nightshades and I'm not as diligent with it as I should be probably but I remember being at a dinner with my family at one point and I was like "no tomatoes for me" and they were like "what's wrong with tomatoes? Tomatoes are really helpful, they are really good for you, they are good for your vision" and they start listing off all these health properties of tomatoes and I'm like "yeah, but not for me".
These things might be healthy in and of themselves if you just break it down and look at the nutrients and the phytonutrients that they have in them. It's the same thing with coconut oil, yes it's a really healthy fat profile and something that most people could probably benefit from but you have to make sure that you are capable of processing it, that your body isn't mounting some kind of inflammatory response to it.
Jonathan: One of our chatters, Lynn said "I can't do anything with any kind of coconut product". Certain people discover that and then you just alter accordingly.
Doug: It's funny because one of the things that coconut is being promoted for now in alternative health circles and even in the mainstream to a certain extent is for Alzheimer's. People are saying because of the fatty acids, because they are converted to ketones so quickly then it's a very beneficial thing. But if that individual is having an inflammatory reaction to it and they have tied Alzheimer's to inflammation then it might be doing more harm than good.
Jonathan: I think that speaks to the benefits that so many people in our circle have seen from switching, first to paleo and then some to the full-on ketogenic diet. A lot of these conditions just improved in due course with that switch. I think that that is a really important first step but every case is different. You might need to go to a doctor and get a shot of cortisol or prednisone depending on what your condition is; if you are really, really suffering. I don't want to rule that out entirely in emergency situations but a good first step is to look at your diet, what you are taking in, make those gradual changes and you will notice an improvement. I can almost 100% guarantee that whatever is going on with you, if you take these steps towards the anti-inflammatory diet that they will begin to improve.
Tiffany: The reason that the paleo diet or the ketogenic diet works is because you are cutting out so many offensive foods, nightshades, gluten, grains and dairy that it helps to heal your gut. If you are eating a standard American diet with lots of carbs and sugars and trans fats and fast food and all that, day after day, month after month, year after year, the lining of your gut starts to break down and food particles seep through. You are not supposed to have food proteins floating around outside of your gut so when those things get outside of your gut they migrate to certain areas and you get some kind of "itis" or "osis". That's really not supposed to be what's happening so when you change your diet, your gut has the chance to heal and the cells in your gut become stronger, they have more integrity and they are closer together so things don't spill out where they should just be staying in.
Elliot: Another important thing to consider is that gut permeability is fluid in the sense that it's constantly changing in response to environmental stimuli. If you are eating coconut oil and tomatoes in January when it's snowy outside, if you look at this from a sort of evolutionary perspective, the body was never designed to consume fruits or tropical oils like coconut or palm oil in the winter; that's a fact. You can't go anywhere in winter in the northern hemisphere and find tomatoes and coconut growing out in the wild. Perhaps to some extent, for a lot of people who can't tolerate these things, maybe there is an aspect of seasonal variability to that.
Perhaps what you can tolerate in the summer in high light cycles may actually drastically differ from what you can tolerate in the winter time. I think what we can try to do is align ourselves with nature in that sense and don't necessarily discount coconut as always being bad for you; maybe you should try it in the summer and then lay off it when it starts to get darker and colder.
Doug: There is probably a genetic component to that too with the idea is that these things are tropical oils. If you don't have genetics that come from the tropics, then maybe they're not the best for your genotype. You can't necessarily say that because I know that there are people who don't have tropical genetics but they can tolerate coconut products, so who knows? Maybe it goes back to ancient ancestry and that sort of thing but that kind of thing might be something that you want to look into as well.
Jonathan: It's definitely at least an indicator. I know we had talked about this before the show and I think I brought this up in another episode of the show as well but there was a case from here in Michigan. There was a guy who went to a doctor and said he had been having some chest pains and he was diagnosed with stage four lung cancer. He was aghast because he was extremely healthy, he was an avid runner, he did a lot of juicing, he did the high fruit, high carb athletic leaning diet and he appeared to be extremely healthy but his doctor then told him that "you are of Scandinavian ancestry so you cannot be eating all of these fruits every single day and not expect it to have a negative impact because the genetics are incompatible." It may not be a one-to-one correlation but it can certainly be a guide I think.
Tiffany: Did you say that this guy was a runner? Like a marathoner?
Jonathan: He was also a runner, yeah.
Tiffany: That is a lot of stress to be putting your body through day after day. When that stress response is kicked up high your body is not going to be in healing mode, it's just going to be in defense mode.
Doug: The long chronic exercise exposure is definitely inflammatory. All exercise is inflammatory to a certain extent, that's why it works; you build your muscle by causing damage to those muscles and then there is an inflammatory response and the body builds up the muscle stronger than it was previously but if you are doing this long cardio marathon type of exercise, your body often can't recover from that inflammation as quickly. That's incredibly hard on the body.
Jonathan: I don't know how this relates to other tissues in the body but I'm guessing it's the same. I had an experience recently where I overstressed my ankle from riding my bike too hard and I hadn't built up to it. We got into the spring here and I was really excited and I took the bike out for a ride and I went out for a really long ride and the next day when I got back I was really, really sore and my Achilles tendon on my right ankle started to swell up really bad. I started looking up Achilles tendonitis and there was that "itis", the inflammation of the Achilles tendon from stress and over-work.
One of the interesting things that I found while I was reading about that is that specifically with the Achilles tendon, when it gets inflamed and breaks down or tears slightly, when it rebuilds itself, the structure of the fibers in the ligaments don't rebuild in the same way. It's kind of like if you have pasta and it's all stretched out nice and neat, that's what a fresh tendon should look like. When it heals itself, it's tangled and it heals back in a mis-configuration form what the original configuration should be.
If you take that example and look at chronic inflammation throughout the body, you have this inflammation and then your body is always trying to repair itself even if you are hammering it with negative things all the time. As it repairs itself it repairs in these mis-configurations and your tissues become knotted; your fascia, the layer between your skin and muscle might be knotted up and you might actually work yourself into a state where it's permanently that way because they have rebuilt themselves in a mis-configuration. So I think that's where a lot of those chronic pain and soreness, especially muscle pain and joint pain, can come from.
But I had really good luck with DMSO, it actually brought down the inflammation and killed the pain just within a few days; that worked really well for me. We were talking about this before the show, it stunk really bad so if you're going to use DMSO for a condition just be sure that you can be away from your friends and family for a few days.
Tiffany: To me it smells like oysters, "who's eaten oysters?"
Jonathan: Another interesting aspect of this I think is the brain inflammation. That was something that was a lightbulb for me when I first learned about it. I'm not sure why I had never made this connection but I remember when I first read about this years ago it was like wow, sure, your brain can become inflamed.
Then there is the lack of blood flow, it impairs the functions of the tissues which then systemically impairs the functions of the signals being sent back and forth and so you can actually hurt your ability to think properly and go throughout the day with proper critical thinking faculties by having an inflamed brain. Of course it is a multi-risk-factor kind of thing, it comes from many different sources. Especially if you get into a case where you are chronically inflamed and have systemic inflammation, it will eventually work its way up into your brain.
There was an article on SOTT here called Inflammation is Associated with Lower Intelligence and Premature Death. They said "The research, recently published in Brain, Behavior and Immunity, used large population-based registers containing data collected over several decades. Inflammation and intelligence were measured at 18-20 years of age in nearly 50,000 young men, and deaths over the following 35 years were recorded.
"Although we knew that inflammation associated with infection or cardiovascular disease could impair brain function, this is the first time that similar associations have been shown in healthy young people," said Dr. Karlsson. "This suggests that even low levels of inflammation can have detrimental consequences for health and brain function," he added."
Elliot: You have got this really tight knit system, it's like a closed system and it's called the blood brain barrier. It's your body's way of basically determining what should and shouldn't cross this particular type of circulation. When you eat something, it gets absorbed by the gut and it goes into the portal circulation, but then your body doesn't let everything into your brain. There is a specific type of circulation that only allows very specialized nutrients and chemicals to enter into the brain.
The blood brain barrier is really specific and it doesn't let that much in. If you have chronic inflammation then this blood brain barrier essentially loses its specificity and begins to allow all sorts of different chemicals into the brain; toxins and pathogenic bacteria. I think it was Nora Gedgaudas in her book Primal Body, Primal Mind where she spoke about how it's been estimated that 90% of people who have gluten intolerance don't actually experience any physical symptoms that they are consciously aware of. They don't experience IBS or diarrhea that would usually be associated with gluten intolerance.
She talks about how for 90% of these people, the symptoms that they experience are primarily neurological so you've got this gluten intolerance and you don't even know about it because you haven't got any overt symptoms. Actually it's mostly affecting the way your brain functions.
Jonathan: I can see how that would be really easy to miss because you are just going throughout the day and you might be kind of bummed out or telling yourself "maybe it's my job or maybe I'm just feeling down today or cloudy so I'm a little tired" and you don't notice that over many days and months and sometimes even years that it's related to gluten intolerance. There might be up days but you just have this general sense of malaise that you have to work really hard to get over.
I think, like we were talking about earlier, a lot of people turn to the diet cravings in order to correct things like that because you eat some bread or you eat some sugar, you drink a lot of coffee, you get that boost and then you feel good for a little while. Then you get home and you wind down for the evening, you might feel crappy for a couple of hours and then you go to bed, you get up the next day and you have cereal, milk, sugar, coffee and start the cycle over again so that you feel ok. So the things that are making you think that you feel better, are actually causing that further systemic inflammation. It's just like a vicious addiction cycle where you get the high, you crash, you feel bad, you sleep, you come back, you take the high again and just keep doing that over and over.
Tiffany: You get so used to it year after year, you think that's just the way you operate and you have no idea that you can actually feel better.
Doug: The brain connection is very interesting too because they've done a lot of studies recently showing that depression is tied to an inflammatory response. They've tied a lot of the issues with depression to inflammation. They've even said that they think that a lot of the psychiatric drugs where they have this mechanism of action that they're assuming goes on and that's why they work; they might actually just have an anti-inflammatory effect and that's why taking some kind of psychiatric drug can help with depression.
Another interesting thing actually is that for years they have been studying St. John's Wort which is an herbal remedy that helps with depression and they've been really stumped on this because it's not a serotonin reuptake inhibitor which everybody assumed it must be if it's helping with depression. So it's like "what is the mechanism of action? It must be a placebo or something like that"; but the fact is that St John's Wort is anti-inflammatory so that's probably its mechanism of action and why people get relief from depression by taking this.
It's really interesting because people load themselves up on these anti-depressant medications and maybe get some relief from it, when maybe they could just be using St John's wort or more likely if they actually cleaned up their diet, cleaned up their toxic exposure, cleaned up the environment, that would probably give them a lot more relief.
Tiffany: The thing with St John's wort and other anti-depressants is I think that one of the things that they found is that they inhibit the production of inflammatory cytokines and if you have a lot of these inflammatory cytokines floating around in your brain, it doesn't regulate glutamate like it should and you have all this glutamate which is an excito-toxin. So your brain is over excited and that can lead to symptoms of depression, so probably that is one of the ways that they work if they do work some of the time.
They did some tests with people who have autoimmune disorders like rheumatoid arthritis or fibromyalgia and things like that, and they found that when they tested their blood, they had higher inflammatory markers like interleukin 6 or TNF-alpha or a C-reactive protein and sometimes when they started on the St John's wort or some kind of anti-depressant medication, they found that those markers went down. That's proof that depression is an inflammatory condition.
Doug: On this topic, but getting away from depression for a second, apparently statins, the cholesterol lowering medications might be effective for the same reason. When they are effective, but they are not nearly as effective as everybody seems to think they are. Everybody just concentrates on the cholesterol numbers; you take statins until you get the numbers within a particular range and then your doctor is satisfied. But for any good effect that they have, what might actually be happening is that they are just an anti-inflammatory and that's why they have any beneficial effect at all. It has nothing to do with what your cholesterol numbers are, it has everything to do with whether or not you are inflamed because atherosclerosis - that "osis" again - it's an inflammatory condition.
Tiffany: So has anybody ever had their C-reactive protein checked?
All: No
Tiffany: I haven't either but that's one of the tests that you can get to see if you have hidden inflammation because it's a marker of inflammation and it's produced by the liver so it attaches on to the dead and dying cells or bacteria and it sends out macrophages to come in and clean up the junk. So if you want to test yourself with a C-reactive protein test, then if your level is over 3mg per liter then you know you have hidden inflammation; if you don't already have symptoms that indicates that.
Erica: Also brain fog. A lot of people I think suffer from that inflammation at a very low level and have no idea because of the brain fog aspect; or headaches. They don't even connect it with the food situation at all.
Tiffany: So if you think that everything that you eat is fine, go out and get a C-reactive protein test and see what it says.
Doug: It's not a bad idea to do that, as we were talking about before, the idea about hidden inflammation. A lot of times people just don't know that they are in this inflammatory state so getting a C-reactive protein test wouldn't be a bad way just to check and see where you're at.
Tiffany: You could do it before you try eliminating certain foods and then do it afterwards and see what the difference is.
Doug: That's a great idea. A little self-experiment. We are promoting this when none of us have done it though. You should, even though we haven't.
Elliot: If someone has got the money to do it then I think it is a great idea to periodically test and do a few different tests as well. You could get your fatty acid ratio tests done.
Tiffany: The omega-6 to omega-3 ratio?
Elliot: Yeah, omega-6 and omega-3 ratio. Theoretically they should change throughout the year. I know there are certain people who recommend certain ratios; it differs but I think it's good to keep a track of that. Secondly, your hormone panels and check out how your thyroid is doing. If you have the money, it's a great idea just to test all of the things that you can as often as possible as you are making changes in your diet as well, because that's a really good indicator and it can give you a good idea of what's going on inside of your body.
Jonathan: I think that part of the bummer about this too is that it's not just the money; obviously you need the money to get the tests done but I think a lot of people are reticent to try to be their own physicians in that way. We have talked about this on the show before, one option is to talk to your doctor if you have a family practitioner or whoever you go to and ask some questions about this. "What do you think about inflammation?" See where their head is at, do they agree that systemic inflammation can cause these things? "Can you help me figure it out?"
If you are not in that kind of a case and if your doctor is just like "here, just take this, take this and don't worry about it." Then you have to learn certain things about your body, you have to get these tests done, do some research, spend the time, learn about the information because I know a lot of people that I have talked to are like "well I'm not a scientist and that is just too much science for me to figure out. I just don't have the time to do that." Because they have kids or activities or whatever.
It's a hard thing to tell people "look, you just need to suck it up and do it" but that is the case. If you want to learn about this, you need to do some research, learn what the terms mean, what the ratios should be, what your levels should be, go through the information and go through that learning process. There is not a way to just get a test that comes back and says "hey, you're good!" or "hey, you're not good and do this..." you need to actually get into the process.
Doug: It's an unfortunate situation because the reason that some people are resistant to doing that kind of work is just because they are in a bad state. They might have some kind of low grade brain inflammation situation going on so the thought of looking through the science and reading blogs and finding out where they are at and what they need to be doing, just that whole process seems overwhelming. It's a tricky situation.
Jonathan: We also have that societal programming too where "I'm not a doctor so what do I know? I'm not trained for this". Yeah, ok so you might not be trained to do a surgery or you might not know the complete human anatomy or have Grey's anatomy memorized or anything like that but there are things that you can learn. You can really learn about your body and at least get the basics about what you should and should not be doing.
Erica: I think it still has to do with having some sort of sensorial experience too; being aware. With the brain fog thing, if you're not functioning at an optimum way, how long do you want to suffer like that? As we were talking about earlier with the gluten intolerance, for me, I never had any physical reactions to gluten but I had chronic headaches; really bad. It got to the point where it was like my quality of life was so bad after a headache that I wanted to change something and it turned out that it was the gluten that was causing the headaches. Just getting off of it, within two weeks they stopped.
I haven't had a headache in years and for anyone that has suffered from migraines, it's extremely debilitating and none of the medication that they give you works. There is still this whole theory about what causes migraines but for a lot of people it could really just be diet. How much do you want to suffer through it is what it comes down to.
Jonathan: That reminds me, I was just listening to another podcast that I listen to on a regular basis and it was an interview with a woman who was a comedian and actress, I'll leave her name out but she said that she had just gotten this new migraine medication from her doctor that was a lifesaver because it knocked out the migraines, and then in the same section she started talking about how great it was to go into binge eating sugar. "I just have a week where I have to eat a lot of sugar and then I feel great"; not making that connection at all with the chronic headaches. It's like saying I have this medication and it fixes it, so I can do whatever I want.
Doug: Unreal.
Jonathan: I think a lot of people are that way and it's not that they can necessarily even be blamed for it, they just don't know. They just don't know those connections.
Erica: Doctors aren't about to give advice on that either. "Hey maybe you should stop eating sugar for two weeks and see if that's the cause?"
Doug: Forever.
Elliot: To be honest, doctors aren't even trained in nutrition. I think the common medical degree only gives a few hour lectures in nutrition so modern medicine is fairly behind, and the way that they view disease is really quite counter-intuitive. Instead of looking at the root cause of something, they tend to just cover up the symptoms but that doesn't really work; as we can see. It's logical and it makes sense to understand the cause of something, correct the cause and then hopefully the symptoms will dissipate anyway. Modern medicine doesn't seem to understand that for some reason.
Tiffany: I was shocked one day when one of the doctors I was working with told one of his patients to avoid dairy! He actually wrote it down in his notes! I was like "what?"!
Erica: He didn't suggest smoking?
Tiffany: They are still anti-smoking. Smoking is the worst thing you can do. Has anyone every had food allergy tests or IgG tests?
Doug: No, I'm planning to.
Elliot: I'm currently in the process of planning that as well.
Tiffany: Well that might be another test to get aside from the C-reactive protein. If you get your IgG tested, that is a delayed allergic response so you might not feel any overt symptoms; say if you eat a piece of chocolate or something, but your body may still be reacting to it.
Elliot: It's generally a good indicator of a leaky gut as well. Even if someone is on a clean diet then if they still have many of these IgG allergic responses to a wide variety of foods then it is quite a good indicator that the gut is still too leaky. Perhaps there are certain things that they can do to alleviate that.
Tiffany: I had a nice experience last night with some French chocolates. I just had one little square and later in the night I started getting a headache and I woke up with not a full on headache but a little discomfort in my head so I went and read what was on the packet of French chocolate and it said "traces of gluten"; so even just a little. I wouldn't consider that a delayed response, it was almost immediate, like three and a half hours and I stared getting a headache; just from that little bit.
Allegedly, even if you have a little bit of gluten it can mess things up for about 6 months according to one article on SOTT.
Jonathan: I think Nora Gedgaudas said that as well. She had mentioned that for most people, but especially for people who have acute gluten sensitivity, even the tiniest amount can last many, many months. I know I have mentioned this before but I am by no means a bastion of diet strictness, but I do my best. I do backslide now and again, and of course every time I do I've got that consistent reminder that "dude, you can't do this". You get messed up for a week or two weeks, you feel tight, you feel fatigued, get headaches, get brain fog and it's become extremely clear to me now over a number of years of really trying to adjust my diet that when I do have reactive substances the sensitivity keeps going up and up and up.
I'm glad for that in a way because the signs are becoming much more clear now, but I feel bad for people who don't have that acute sensitivity to the reaction itself because you don't notice. Like we were saying, sometimes it's not like your neck is immediately going to seize up for a lot of people, or you're immediately going to feel tired all day or anything like that. You just have these small symptoms like brain fog and things that build up over time, and you start to believe that's just the way things are; that's just my body, it's just whatever condition I have and there is really not much I can do about it.
Part of what we are trying to do with this show is help people understand the diet and health connection because unfortunately even though a lot of progress has been made in this area, it's still not widely understood by the general population I think; that really specific connection between your health and what you're eating. We still have this unfortunate programming that my health is connected to the medicine I take and I take the medicine and I try to fix the thing and then I eat whatever I want. And that's just how it goes for a lot of people.
Doug: What I was finding when I first started changing my diet and when I would have some situation where I did backslide, often when I was out for dinner with co-workers or eating at a family celebration or something like that and I would eat something bad, I started to make a connection which was that I would have more physical body type issues that you would never necessarily connect to what you are eating. So for me at one point I was bending down to put laundry into a washing machine and all of a sudden I twinged out my back. I was like wow; why did that happen?
That's so crazy. I was in pretty good shape; I was exercising regularly but I had this back issue. I healed from that and it took a couple more times for that to happen before I started to connect it to going off the diet and eating bad things. It's not like I went back to eating bread and cheese or anything like that, it was just maybe too many potatoes or something like that.
It took a long time for me to make that connection. I would have this injury that shouldn't have really happened and I tied that to what I had been eating.
Elliot: The gut is basically the body's first line of defense. In biology textbooks it will say that your skin is the first line of defense but essentially your gut is in direct contact with the environment and so if you're ingesting something that irritates your gut, then that is really the easiest way for something to get into your body or cause problems. It hasn't been well established in mainstream medicine but it's coming out now and the research is really showing that your gut is the most important component in maintaining a healthy immune system and health.
Erica: Another unknown factor that people might be dealing with, especially a lot of our listeners who have been on the diet for a long time and are still having inflammatory responses; there was a great article on SOTT about heavy metals and inflammation and how they could be silent killers.
They say that "due to the nature of heavy metals, important nutrients are blocked from absorption and assimilation. As observed by Dr. Hanshew, "the activity of the enzymes is also dependent upon nutrient co-factors such as Magnesium and Zinc. Toxic heavy metals, such as Mercury specifically block the absorption and assimilation of these nutrients and thus can negatively affect the enzyme activity."
They talk about how mercury is super toxic and it blocks this absorption. Maybe Doug or someone can go into a little bit more of the science behind that, but if you can detox your body from heavy metals it's essential to dealing with that inflammation state. They talk about heavy metal chelators like chlorella, zinc and zeolite. Chlorella binds to heavy metals like mercury, arsenic, cadmium and lead and safely escorts the toxins out of the body; all without risk of re-absorption in the digestive tract. Do you have any more insightful information on that Doug? What the heavy metals actually do, because I know for some of our listeners, people have had the heavy metal tests and some people are definitely suffering from heavy metal toxicity.
Doug: I think that one of the big things is that when you do have toxic heavy metals in your system, it can interfere in a lot of different ways. It said in the article that it interferes with different enzymes and you need enzymes for every process that goes on in your body. Just by interfering with these different enzyme systems you can have issues with inflammation come up.
One of the things it said in the article, was that it interferes with the prostaglandins in the body. They are almost like hormones, but are not quite hormones and there are inflammatory ones and there are anti-inflammatory ones. You need to have a good balance of both, but by having heavy metals in the system, the body will lean more towards having the inflammatory ones and not have the anti-inflammatory ones for shutting it off; that's a big problem. The whole heavy metal issue is actually very overlooked in our society right now, I think.
Tiffany: Heavy metals are some of the things that can break down the blood brain barrier. I think that has been implicated in autism; with the aluminium or mercury in the vaccines.
Elliot: Heavy metal toxicity also messes with the conversion of omega-3 and omega-6 fatty acids in the cell membrane. You are meant to have this specific ratio between omega-3's and omega-6's but if you have heavy metal toxicity then your body essentially doesn't know what to do with those fatty acids and you build up an excess of omega-6 fatty acids in your tissues and in your cell membranes and that in-and-of-itself triggers a cascade of inflammation.
It says here in this article that "Toxic heavy metals can also shift the equilibrium activity of Delta-6 desaturase to increase the production of GLA, DGLA and AA and decrease the production of EPA, DPA and DHA." So EPA, DPA and DHA are omega-3 fatty acids and they are essentially anti-inflammatory whereas the others are pro-inflammatory so if you are toxic with heavy metals you are basically just increasing the inflammation by ten-fold in your body.
Tiffany: So it's good to do those heavy metal detoxes. Maybe a few times a year. You can use chlorella, cilantro and zeolite. What's that pill that chelates heavy metals?
Doug: DMSA?
Tiffany: Yeah, DMSA. Do one of those maybe two or three times a year just to keep your body in balance.
Jonathan: I think you need to be cautious with that too; look up the protocol, make sure you are doing it in the right way because especially if you are overly saturated with a certain heavy metal or a combination of them. If you flush it out too quickly, I guess I'm not aware of any lethal side effects to that but you can certainly give yourself a really acute illness.
Tiffany: Make sure that you re-mineralize afterwards because it can deplete the good minerals from your body. If you do a cycle, make sure you follow the directions to the letter.
Erica: We spoke a little bit about that in the iodine show too; the iodine can also release those heavy metals stored in the brain. For some people, myself included, it can be a pretty unfriendly experience; very depressing.
Elliot: Another interesting thing about iodine is its association with DHA. There is an article on SOTT called Harvard and USC Scientists Show how DHA Resolves Inflammation. It's this study that was published in the FASEB Journal and what this showed was that DHA essentially inhibited or decreased inflammation in the body.
Now DHA is a common component of fish oil and when people talk about omega-3 fatty acids and how good they are for the brain and how good they are for anti-inflammation, they are talking about DHA and EPA. DHA has this amazing effect on inflammation, it drastically decreases it but one of the interesting things about iodine is that it basically acts to protect DHA in the body. So when you ingest DHA it's a polyunsaturated fatty acid so what that means is that it's very prone to degrading, it's very prone to something called oxidation.
What iodine does to DHA is it essentially protects it, it acts as an anti-oxidant and this is why you find DHA and iodine in fish. Essentially iodine, aside from all of the other amazing qualities, also acts to protect this vitally important nutrient, DHA, in the body.
Tiffany: When you have an infection, you have these white blood cells and macrophages that come in to eat up the infection. If you have ample DHA, it won't all get used up because the macrophages will use the DHA to produce something called a maresin. The maresins act like a switch to turn inflammation on and off so if you have enough DHA you can produce these maresins, and it can turn off the inflammatory response.
Jonathan: If I'm not mistaken cold therapy is also really good for DHA as well, right?
Elliot: Yes, cold therapy is really good for maintaining DHA stores. Two of the most important things for maintaining DHA are that one, it should be gotten in adequate amounts in the diet and that's really important. I know there is some DHA in grass-fed meats.
Tiffany: Lamb is high in DHA.
Elliot: Lamb is very high in DHA, but really the highest sources of DHA are found in natural fish foods; oysters have an extraordinarily high amount of DHA; cold water fish. You can take a supplement form of DHA but I would say personally, it would be a better idea to take it in its natural form because you also have the co-factors like iodine and we know that iodine protects DHA in the body from oxidation. It also has selenium which works in conjunction with iodine so it can get quite complex.
The main important thing to remember is to eat enough DHA in the diet but secondly, what we need to remember is that exposure to blue light actually degrades DHA in the retina. Your body can't store that much DHA so its main concentration in the body is actually in the eyeball. When you are exposed to blue light, what this actually does is degrade that DHA in your eye so in order to maintain DHA levels it would be very important to limit your blue light exposure.
You can get these amber tinted goggles; these are really important especially when it gets dark or when you are looking at a computer screen. That's something you can do to try and maintain your DHA levels.
Tiffany: If you are going to take fish oils, you have to be very careful of the kind that you get because some of it is probably already oxidized by the time that you get it. If you are going to try and do it because for some reason you can't get fresh fish or sardines or oysters, try and get it when it's produced in the winter time and have it sent to you during the winter when it's cold. It should be in a dark capsule in a dark bottle and it should be refrigerated; natural is best but if you are going to try and supplement with fish oil just make sure you get very good quality.
Elliot: Also, another great alternative to fish oil which I would probably recommend over fish oil is krill oil. Krill are basically these small shrimp-like creatures; they are not as prone to oxidation. There have been studies done on krill oil when compared to fish oil and it was shown that krill oil withstood much longer periods in heat and in the light. So really if you can afford it, it's a little bit more expensive but krill oil is probably the way to go, in my opinion.
Jonathan: I wonder if there was a way to find out where the oil actually comes from; like what region because I would be keen to avoid fish oil that came out of the Pacific Ocean due to Fukushima. I remember reading a little while ago that a lot of the dead fish that had turned up from the Gulf oil spill in the Gulf of Mexico had actually just been harvested and then taken for fish oil. I can't verify that right now so I don't want to try to fear-monger but I'm saying, if there is a way for you to discover what the source and the quality of these oils are, sometimes it requires paying a little bit more, but sometimes you just need to call the company and be like "hey, where do you get this from?"; if you can get through to them in that way.
Erica: They are making a lot of fish oil with GMO oils too so if you go to a Costco or a Sam's Club, I wouldn't recommend buying their fish oil. As you said, read the ingredients because it will tell you right on there. It won't say GMO oil but it will say canola or soy bean which you can just assume is not good.
Jonathan: Talking about the heavy metals issue, I wanted to say that clay is really good for that and I have done a bit of research. I wouldn't consider myself an expert but it's pretty affordable, it's really easy to take and it's an extremely effective chelator for heavy metals. If you look into French Green Clay, bentonite, montmorillonite and different combinations of those, there are specifically blended clay combinations that are made for internal usage that you can get online.
If you are going to look into that, be really careful not to get cosmetic green clay because a lot of that has aluminium added to it. You cannot just order some French Green Clay and take it internally; look into it and make sure that it's pure and has no additives and preferably that it's intended for internal use; but that it's a really effective chelator.
Tiffany: Speaking of inflammation in general, yoga has been found to decrease amounts of inflammation. They did a study where they had people do the yoga breathing for just 12 minutes a day for 8 weeks and they found that when they tested their blood they had lower levels of C-reactive proteins. So what's so great about yoga? It's very relaxing and that's one of the good things about it.
Erica: There is definitely this idea that the vagus nerve controls intestinal inflammation. There is an article on SOTT for those who are interested and for anybody who has tried the EE program or those regular practitioners; the relationship between stimulating the vagus nerve and reducing inflammation in all of the organs of the body. Also acupuncture can be anti-inflammatory by stimulating the vagus nerve and its effect on these microphages that you were talking about Tiffany; that result in tissue inflammation.
Then, wait for it, nicotine is anti-inflammatory by acting on the acetylcholine receptors normally responsive to acetylcholine released by the vagus nerve. Do you guys have any more to share on that? For those who have practiced the EE breathing or this yogic breathing that Tiffany was talking about; the Ujjayi pranayama; the constriction in the throat in that breathing through the nose, keeping the throat slightly constricted stimulates the vagus nerve in the throat and it really helps with inflammation in the brain for sure.
There was an article on SOTT which was very short, easy to read, about reprogramming inflammation with meditation. They did a study at the University of Wisconsin showing that meditation can actually affect the genes that cause inflammation. They measured the effects of day of intensive mindfulness meditation in a group of experienced meditators and compared them with those of quiet non-meditative activities by a group of untrained volunteers. After 8 hours of meditation the researchers found altered levels of gene regulating compounds and reduced activity levels of the pro-inflammatory genes in the experienced meditators. These changes were correlated with faster physical recovery from a stressful situation.
They also reported that these findings are the first to show that meditation can inhibit the production of proteins by some genes that cause inflammation and noted that at the study's outset there were no differences in the genes tested in both groups. They also reported that positive changes were seen in genes that are targets of anti-inflammatory and pain-killing drugs. Basically practicing breathing exercises like we share in the Éiriú Eolas program and meditation exercises consistently will help slow those inflammatory responses in the brain and in the body.
Tiffany: So a lack of stressful thoughts, like slowing down the chatter in your brain can turn off genes that make you inflamed.
Erica: Yeah and it kind of goes back to our show on the placebo effect. When you have eaten some inflammatory foods and your knee's aching or your body is aching or you have a headache, you start to stimulate your vagus nerve by practicing these breathing exercises and they calm that inflammatory response in your system.
I like to have a visualization of it, like if I ate too much mashed potato and my knee hurts I'm going to focus my breathing on my knee and let go of that pain, if that makes sense. Do any of you have any experience with that?
Jonathan: Not specific experience with an actual condition. I can say that I generally feel better when I am able to relax when I do the Éiriú Eolas program overall. I guess for me it manifests as, this may sound strange, but I get a lot of movement in my joints, especially in the upper part of my neck and in my knuckles and sometimes in my hips. By movement I mean they will pop and crack a lot and my chiropractor told me that that's not always bad; in a way it's good because it's a sign that the tissue around the joint is not inflamed, allowing it to move where it needs to go.
Tiffany: I have noticed that. I noticed that too when doing the meditation, I feel the need to stretch more. Not during the meditation but afterwards and during the day I do notice that I hear my joints popping more. Before I didn't really feel the need to stretch a lot but now I do stretch a lot, I can hear the popping and clicking sometimes; that makes sense.
Jonathan: I have definitely noticed that when I'm not inflamed, a clear sign to me is that I will get the popping and the cracking, most often in my neck. Obviously you don't want to lean on your head, you don't want to put sideways pressure on your head but even just leaning my head slightly to the side there will be some tension and then it just goes pop!
When I'm inflamed that doesn't happen. It's like you can't get it to move. The advice from the chiropractor was that it's likely a marker of inflammation because the tissue around the joint is puffed up and it's not letting it move correctly.
Tiffany: So the stiffness goes away. I have noticed too with the meditation that my mood is a lot better. I don't have as many "blah" days or dark thoughts, that's another sign of not being as inflamed, I suppose?
Erica: Definitely. It's really remarkable, especially with the EE program, even after just 10 rounds of the pipe breath in through the nose, out through the mouth, how you get this sense of calm that comes over the entire body. Especially if you are in a stressful situation and you start to notice everything tense up; your jaw or your shoulders; in your body you get these physical sensations of stress. You just know to use that breath to stimulate that vagus nerve to stop or at least try and mediate that inflammatory response.
Tiffany: Another good thing about the meditation is that it helps you sleep better, and sleep or a lack of sleep can cause inflammation. They did a study where they studied people who stayed awake from 11 p.m. till 3 a.m.; just partial sleep problems can cause an increase in something called nuclear factor-B which is a signal of inflammation. So just after being awake for that period of time during the night, for one night, that nuclear factor-B went up. That just shows how important it is to have regular restful sleep. Sleep enough, sleep in a dark room, don't be too hot, just be comfortable and get at least eight hours or however much your body needs so when you wake up you are feeling rested and not still a little groggy and tired.
Erica: Definitely, with a lack of sleep you start to notice the cascade of all these inflammatory responses. It's almost like the immune system is taking a hit and then everything is a little bit more susceptible.
Tiffany: You are more susceptible to colds and flus and other infections, plus the brain fog that you get when you don't get a good night's sleep and you start forgetting things or dropping things and not being able to think straight.
Elliot: If people do actually have issues with their sleep, then one thing to try would be to keep the window open at night time and preferably throughout the whole day, even if it's cold outside. Another thing is to try to sleep naked, because if you are wearing underpants or a T-shirt or anything like that then the body finds it hard to lower the temperature. The body needs to regulate the temperature because at night it's signaled to produce melatonin, so when you sleep it's the lowest body temperature that you are going to have in the whole day.
Your body needs to lower that temperature, it's really important that your body can lower that body temperature. If you are too hot or you have got clothes on then your body finds it a lot harder to do that and sometimes it can't produce those vital chemicals that do facilitate a restful night's sleep.
Erica: As we shared on a previous show, sleep issues plague many people and it's good to notice when you get out of balance and you start to lose sleep and how things can really start to go downhill from there. I agree with Tiffany, the meditation before bed is essential to slowing the mind down, slowing the body down, preparing for relaxation; you have got to do it!
Jonathan: The blue light issue that Eliot brought up too. I noticed, not necessarily all the time but there are specific times where I notice if I am using a computer right up until the point where I go to bed, I just go from that, turn it off and go to bed, it takes me a lot longer to fall asleep.
Tiffany: You should get some of those glasses.
Jonathan: I have been thinking about that.
Tiffany: The blue blocker glasses.
Erica: And not having that electrical stimulation at least an hour before bed. Turning everything off, not reading on a tablet, maybe reading a book; switching your mind into a different state.
Jonathan: There is a program for anyone who uses Windows, I'm not sure if it exists for Mac or for Linux but it's called Flux. It synchs up with your clock and the time zone and the light changes and then as the sun begins to go down and it gets darker, it will shift the color of your screen to a little more of a red tint and take the blue out of the screen; it's not a cure-all but it does help.
Elliot: Ever since I started wearing blue-blocking glasses I found my sleep transformed. It was really amazing because I thought it was just fairly normal to wake up quite groggy every single day. As it started to get dark I would stick on my blue blocking goggles and I actually found that for the first time in my life I actually felt tired by about nine o'clock. That was really strange for me because I was one of those night owls who could happily stay awake until 4 a.m. every night but as soon as I started wearing them it was really quite amazing.
Jonathan: It's certainly something to try out. Mikey in the chat says that for listeners who might not be in the chat, that for Linux there is also a program called Redshift that works quite well for changing the color tint of your screen.
Tiffany: So what else can we do to relieve inflammation? Mild to moderate exercise? Not marathon running?
Jonathan: Meditation, relaxation, specifically the Éiriú Eolas breathing program. Diet changes, detoxing heavy metals to the best of your ability.
Erica: Turmeric is a great one too, especially for body inflammation. A few of our chatters talked about using it for certain ailments in the shoulders, knees, hips or the lower back. You can even put turmeric in a massage oil, it's not the cleanest, it might turn your skin a little bit yellow but actual physical application of turmeric in addition to taking it internally. There are numerous articles on SOTT about the anti-inflammatory properties of turmeric.
Jonathan: MSM for joint problems; it's methyl-sulfonyl-methane. You will find it under the name MSM. That is quite effective for systemic inflammation but also specifically for joints and for cartilage. I've had good experience with that.
Tiffany: I have experimented with that and I was wondering why I was having heart palpitations all of a sudden. So again, as with everything you have to try it for yourself and see if your body likes it, even though it might be hailed as a wonder supplement; try it for yourself.
Erica: Magnesium, magnesium bath. Do your meditative breathing in the bath with magnesium.
Jonathan: Epsom salts are pretty affordable and usually easy to find at a supermarket so that's something that I think most people can get their hands on.
We have covered a lot of good information here today and I think we are nearing the end of our time so let's go to the pet health segment for today; Zoya has a little talk for us about how veterinarians make diagnoses. That sounds like some pretty interesting information. We will be back after this.
Zoya: Hello and welcome to the pet health segment of the Health and Wellness Show. My name is Zoya and today I would like to share with you my thoughts on why many people find medical and specifically the veterinary professions so fascinating, and how veterinarians think can be related to the way we all think and solve problems in our everyday lives.
Most of us like detective stories, many of us, when we were still children, played all kinds of games where we imagined ourselves being spies, explorers or great adventurers. As a race, we like mysteries and riddles. therefore it isn't surprising that some of us would like to be able to solve riddles in our professional life as well; it's not always easy.
In fact, as a student and almost full-blown veterinarian doctor, I can tell you that there is a huge difference between theoretical knowledge and practical experience. High grades don't heal that's for sure! And actually the fact that we have this saying "doctor from God" for example, indicates that medicine is like another form of art. It's a talent that in some cases no amount of training is able to imitate. It happens when doctors use their intuition or some other abilities that are not overly systemized.
What is behind the magic of correct diagnosis and what can we learn from it about the way we think and approach other problems? After all, veterinarians are human too. Here are some ideas that I took from a fascinating article titled Case-based Clinical Reasoning in Feline Medicine - Intuitive and Analytical Systems. But first, please remember the following main concepts, there are two main forms in which a brain does its thinking, there is System 1 thinking which is immediate and unconscious and System 2 thinking; thoughtful and analytical.
The article poses a question, if in this era of evidence based veterinary medicine where accuracy and objectivity have perhaps become valued more than skepticism and open-mindedness, is it heresy to use intuitive pattern recognition to diagnose diseases in practice? Many who advocate this exclusive use of an analytical, problem orientated approach would answer with an emphatic "yes" believing the thought processes of pattern and recognition to be fraught with inaccuracy and cognitive error.
While the sometimes spectacular failings of intuitive reasoning cannot be denied, it is accepted that experienced clinicians, especially elite clinicians, find it difficult not to engage in intuitive reasoning from the moment they first see the patient and its owner. Furthermore, if intuitive pattern recognition or other forms of intuitive reasoning are used more effectively through conscious refining, this will save time and money for clients by sharpening diagnostic accuracy and reducing unnecessary tests and procedures.
Moreover, intuitive reasoning, especially pattern recognition, comes naturally and intuitively to many clinicians, even if they cannot appreciate how and why it occurs. Is there room for using both approaches? The question is truly rhetorical as there is a wealth of evidence from the psychology, economics and medical literature to establish the power of using both cognitive approaches.
So this article argues that there is merit in using both intuitive reasoning and pattern recognition, being the most well-known form of System 1 thinking and the analytical, problem oriented forward reasoning approach as a trained form of System 2 thinking. The bottom line is that the most optimal solution is to combine both systems. It means that whenever intuitive System 1 thinking is employed, it should, where possible, be tested and backed up with evidence provided by analytical System 2. The question is, why do some veterinarians favor one system over the other in the way they think about clinical problems?
The short answer is we don't really know. But perhaps inherited and acquired personality traits play a key role in dispositional tendencies. It was once suggested that individuals inclined to use more of the right side of the brain feel more comfortable with intuitive thinking while those who use the left side of the brain feel more comfortable with the analytical, problem orientated diagnostic approach that the System 2 thinking has to offer.
However, like most good stories, it has been refuted through further research, particularly neuro-imaging studies. What is accepted however is that those of us who do favor System 2 thinking like using lists and organizational charts while System 2 thinking is criticized for being costly, time consuming and stifling of creativity, it is probably more protective of mistakes being made in the reasoning process so long as the detection or perception component is not flawed.
The novice clinician, like me for example, will find System 2 thinking tiring and laborious but fruitful in terms of developing understanding and expertise about disease presentations. Importantly, once a newly encountered disease condition has been diagnosed using System 2 thinking, this stored case information, either as a simple pattern or a more complex illness script, becomes accessible through an unconscious System 1 thinking mechanism the next time such a problem is encountered.
Central to System 2 thinking is the ability to consciously resolve a large number of signs and findings into a small finite number of mini-patterns or problems. Generally, there should be fewer than five problems. It is usually the fact that the mind working on short term memory usually struggles with more than five so that the amount of information to be processed is not too overwhelming.
By contrast, intuitive System 1 thinking using pattern recognition is about the emergence or recognition of complete patterns; or sometime partial patterns through unforced or unconscious thought. This form of adaptive reasoning asks the question sometimes unwittingly, what is the most plausible explanation for the pattern? Although it still comes up with a hypothesis, as does System 2 thinking. It does it in a way that relies on long term memories of past cases and often ignores what is regarded as useless data, referred to by engineers or neuroscientists as noise.
In essence, it is a recall of one or more past experiences, especially your own clinical experiences but also from texts, reading or seminars attended. It relies on key aspects of the history which are often interconnected with observation of the patient, physical findings and characteristic diagnostic imaging or laboratory findings.
These triggered past experiences may be simple patterns or may take the form of extended case histories, referred to as illness scripts. Such scripts are strongly suggestive of either a final diagnosis or a fruitful avenue for further investigation through an established hypothesis.
There is much more fascinating information in this article and I am actually not done reading it; there are three parts; but you get the idea. Also, some of you may be more able to see and recognize the same concepts discussed in books like Blink or Thinking Fast and Slow for example. If so, then you can understand my excitement about this material. It is indeed very exciting to see that veterinarian specialists utilize pattern recognition and use similar concepts while treating our furry companions, so I hope that it was interesting and that's it for this segment, have a nice weekend and goodbye!
Jonathan: Alright, thanks Zoya, that was great; definitely worth looking into the System 1 and System 2 thinking. Really interesting correlations there with how they make diagnoses, that's also very helpful for determining how we think and where our impulses and things come from.
For the topic on our show, we can tie that in to how you make choices about what you are eating and where your cravings come from. You can use these techniques to determine "am I thinking instinctually, quickly or am I actually analyzing what's going on in my head?"; making smart choices based on that."
Today for the recipe, we haven't got a specific recipe but more-so of a technique I was playing with this last week which is kind of fun. It may not necessarily be fun for everybody but for me, I like to play with food. I noticed that when I was making burgers, a lot of the time in the pan, depending on whether or not you grill all the time or not, but if you make burgers on the stovetop they will puff up and get really roundish and sometimes they can dry out that way. Other times they can make it hard if you are trying to stack, like if you want to put bacon and avocado and stuff on top of the burger it can make it hard to eat because then everything will just fall apart on your plate and you might as well just mash it all together.
I got curious and looked up how to make skinny burgers and it's actually pretty simple but it was kind of a lightbulb for me. You take the ground beef, make it into a ball maybe about twice the size of a golf ball depending on how big you want your burgers to be, get the pan really hot, put some oil, bacon fat or butter in there and then put the balls of ground beef in the pan, just slightly compress them so that they are not all the way compressed and let them cook on one side for about a minute. Then flip the balls over to the other side so that the fried side is up and you will have a portion of that side of the sphere that's cooked.
You flip them over and as soon as you flip them over you mash them down. I know that this is antithetical to a lot of burger connoisseurs; you are not ever supposed to mash burgers but they actually turned out really good. So you flip them over and you mash them down really hard and make them really flat and that previously cooked side of the ball of the ground beef actually holds them together and prevents them from breaking apart into a bunch of pieces.
You mash them down and you cook that for about a minute on that side, then flip them back over to the first side and then cook them for about another minute. What you end up with is actually quite juicy, thin burger patties and that can make it easier for stacking other things on top of the burger depending on how you want to put it together. I usually like to have mine with some bacon, avocado and aioli and maybe some sprouts on top. It makes it a little bit easier to contain that whole thing and then you can eat it with a knife and a fork.
Tiffany: That's a god technique.
Jonathan: It actually works really well and you would think that they would be kind of dry and burnt but they are not. If you cook them for that very short period of time they come out really juicy.
Erica: Another thing that you can do to not have dry burgers is mix a little bit of ground pork in with the beef; and bacon fat.
Jonathan: I have had fun doing that with butter. Basically just cube some cold butter and then really work it into the ground beef with your hands when you are mixing it up.
Erica: Butter burgers are better!
Jonathan: I am also currently experimenting with using ground pork rind. We had done some pork rind flour recipes in the past for making baked goods with ground pork rinds so that you get a very, very low carb baked good that you can make. I have been trying to use gelatin as an emulsifier as opposed to xanthan gum or anything else and it works really well. I'm trying to work up a recipe for that and hopefully we will be able to do that next week. So maybe you can have buns with your burger.
Tiffany: We have had pork rind buns, they turned out pretty good; we put onion flakes on it.
Erica: You can also use lettuce as a bun but it's not quite as fun as the pork rinds.
Jonathan: Alright well that's our show for today. Thanks to all the chat participants for tuning in and for taking part in the discussion and to our listeners. Just want to remind you to check out the Truth Perspective show; is the Truth Perspective on tomorrow?
Tiffany: No, they are going to merge onto Sunday.
Jonathan: That's right, so the Truth Perspective and Behind the Headlines are merging and will now be aired on Sunday at noon Eastern time. No show tomorrow, but be sure to tune in on Sunday and there are some things going on behind the scenes here at SOTT Talk Radio, we are working on some new show ideas so be sure to stay tuned. We may have other shows coming into the mix and hopefully even possibly some multi-lingual shows for our overseas listeners; that would be really exciting. Check out radio.sott.net on Sunday and of course not everybody is in the US Eastern time zone so the correct time zone will be displayed on radio.sott.net wherever you are so just be sure to check that page out and check out the show! We will be back next week, thanks again everybody and have a great weekend!
All: Goodbyes



[Link]