The severely brain-injured patient, who is now 38, was unable to communicate, swallow or make co-ordinated movements for six years, before doctors revived him from this mini-mally conscious state (MCS) with a revolutionary therapy.
Since his skull was implanted with electrodes to stimulate a deep-lying and undamaged part of his brain, he has improved so dramatically that he can now feed himself, brush his hair and recognise and talk to his parents and doctors.
"My son can now eat, sleep, watch a movie without falling asleep, he can drink from a cup, he can express pain, he can cry, and he can laugh," his mother said.
"He can say, 'I love you, Mommy'. God bless those wonderful doctors who believed in my son, and gave their time and effort to help my son."
One of his most impressive achievements has been to say from memory the first 16 words of the Pledge of Allegiance, which is recited daily by American schoolchildren.
The transformation achieved by the deep brain stimulation (DBS) technique, which is already used to treat Parkinson's disease and some mental illnesses, has raised hopes that it could offer a way back to consciousness for many people with similarly serious brain damage. While there are few reliable figures for the number of MCS patients around the world, doctors estimate that the total runs to hundreds of thousands. The research team, which has published its results in the journal Nature, will now start the first formal clinical trial on 12 American patients.
|
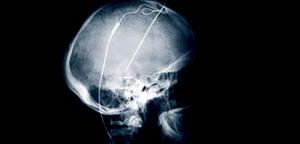
| ©Cleveland Clinic/PA |
| Deep brain stimulation electrodes were implanted into the skull of the patient who was suffering from severe brain-injuries |
"We hope that the first use of DBS to treat patients in an MCS marks the beginning of a significant period of innovation in our approach to traumatic brain injury," said Ali Rezai, Professor of Neurosurgery at the Cleveland Clinic in Ohio, who implanted the electrodes.
Joseph Fins, Professor of Medicine at the Weill Cornell Medical Centre in New York and another team member, said: "This innovative procedure holds the potential for patients to recapture a lost personhood as they regain an ability to communicate through a prosthetic device that helps them participate in the human community.
"If this is replicated, its success could usher in a whole new era for the treatment of patients in MCS. Any intervention that can unlock the neurological potential of patients in MCS should have us reconsider how we care for these individuals."
MCS patients differ from those in a persistent vegetative state (PVS) in that, while they are so brain-damaged as to be mostly unaware of their surroundings, they show signs of consciousness and may communicate with simple signals or respond to stimuli. They retain capacity in parts of the brain that process higher cognitive functions, which are inert in PVS.
It is not thought that DBS would benefit PVS patients such as Terri Schiavo, the Florida woman allowed to die in 2005 after a legal battle between her husband, who wanted her feeding tube removed, and her parents, who wanted her to be kept alive.
The patient's improvement after DBS treatment was almost immediate. His mother had previously been told that, if her son survived, he would be "a vegetable for the rest of his life".
She said: "Each time I visited my son in the nursing home on my way home, I would cry, as it's so hard for a mother to see her son like that, and I'd pray for a miracle . . . In 2005 it happened, the opportunity came.
"I can imagine what other families are going through, when they come back from the war with all sorts of injuries, and I would like to say to them, 'Don't give up hope. There is hope'."
Electrodes used to stimulate key areas
- The first patient to be treated with DBS suffered brain injuries in a robbery and assault in 1999
- He was fed through a tube, could not speak and was barely able to communicate
- Brain scans showed that key regions still functioned and, in 2005, his parents approved the treatment conducted by Professor Ali Rezai and his team
- Two electrodes were inserted through the skull to stimulate the thalamus, a part of the brain that arouses other important circuits
- Over six months, they were switched on and off, in a random pattern, so doctors did not know when he was being stimulated
- The improvement was almost immediate
- The implants now work permanently: they are switched on for 12 hours and off for 12 hours, to allow him a normal asleep-awake cycle



Reader Comments
to our Newsletter