In my last two articles, I discussed the history of salt in the human diet and the physiological need for salt. Many proponents of the Paleo diet suggest limiting salt based on evidence of low salt intake during the Paleolithic era. This limitation meshes with recommendations made by various health organizations, such as the USDA and the American Heart Association, who suggest limiting sodium to at least 2,300 mg per day and even as little as 1,500 mg per day. (1, 2) And if our Paleolithic ancestors ate a low salt diet, then it certainly must be healthy, right?
Not necessarily. Recently, evidence has been mounting against universal salt restriction guidelines. A low-salt diet may cause serious health consequences and higher overall mortality, especially in the presence of certain chronic health conditions and lifestyle factors. In this article, I will discuss scientific evidence that contradicts salt restriction recommendations, as well as potential health risks of consuming a diet too low in salt.
Serious health consequences of long-term salt restriction
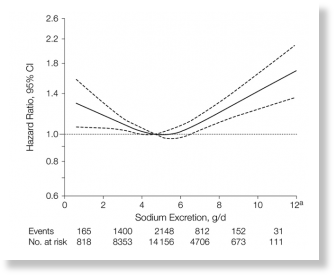
Another 2011 study confirmed this observation; not only was lower sodium excretion associated with higher CVD mortality, but baseline sodium excretion did not predict the incidence of hypertension, and any associations between systolic pressure and sodium excretion did not translate into less morbidity or improved survival. (4)
Low salt diets contribute to an increase in hormones and lipids in the blood. A 2012 study in the American Journal of Hypertension found that people on low-salt diets developed higher plasma levels of renin, cholesterol, and triglycerides. (5) The authors concluded that the slight reduction in blood pressure was overshadowed by these antagonistic effects, and that sodium restriction may have net negative effects at a population level.
In addition, low sodium intake is associated with poor outcomes in Type 2 diabetes. A 2011 study showed people with Type 2 diabetes are more likely to die prematurely on a low-salt diet, due to higher all-cause and cardiovascular mortality. (6) Additionally, a 2010 Harvard study linked low-salt diets to an immediate onset of insulin resistance, a precursor to Type 2 Diabetes. (7) These studies call into question the appropriateness of guidelines advocating salt restriction for patients with Type 2 diabetes.
Restricting salt is also problematic for athletes, particularly those participating in endurance sports. (8) Recent studies have shown that endurance athletes commonly develop low blood sodium, or hyponatremia, even in the absence of cognitive symptoms. In the 2002 Boston Marathon, it was found that 13% of 488 runners studied had hyponatremia, and studies of other endurance events have reported the incidence of hyponatremia to be up to 29%. (9, 10, 11, 12) While the majority of these sodium deficient athletes are asymptomatic or mildly symptomatic with nausea and lethargy, severe manifestations such as cerebral edema, noncardiogenic pulmonary edema, and death can occur. (13) It is extremely important that athletes engaging in high intensity or long duration exercise be sure they adequately replace the salt lost through sweat.
Salt restriction may be especially dangerous for the elderly. Elderly people with hyponatremia have more falls and broken hips and a decrease in cognitive abilities. (14, 15) Hyponatremia is a common finding in the elderly, with an especially high prevalence in those with acute illness. (16) This is another population at risk for serious health consequences due to universal sodium restriction.
Why is the government still recommending salt restriction?
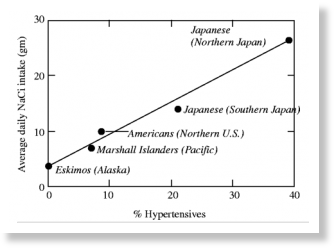
However, when Intersalt researchers investigated this possible association, while controlling for confounding factors, the correlation between blood pressure and salt intake almost disappeared. (22, 23) For some reason, this contradictory evidence is still being used today to justify restricting salt intake.
In 1998, Gary Taubes wrote an article for Science magazine highlighting the clash of public policy with controversial scientific evidence for salt reduction. (24) He described how most of scientific discord over salt reduction has been overshadowed by the public attention given to the benefits of avoiding salt.
As Taubes explained over a decade ago, "the data supporting universal salt reduction have never been compelling, nor has it ever been demonstrated that such a program would not have unforeseen negative side effects." The 1988 Intersalt Study, designed to resolve contradictions in ecological and epidemiological studies, failed to demonstrate any linear relationship between salt intake and blood pressure. Now, in 2012, we have data that suggests long-term salt restriction may pose serious risks for much of the population. Yet major health organization guidelines still recommend the restriction of salt for all Americans, regardless of blood pressure status.
In short, there is a healthy range of salt consumption for most people. When eating a whole foods diet, most people tend to consume an appropriate amount of salt simply due to an innate preference for saltiness. In fact, the consumption of salt around the world for over two centuries has remained in the range of 1.5 to three teaspoons per day, which appears to hold the lowest risk for disease. (25)
Our bodies may have a natural sodium appetite through which our ideal salt intake is regulated. By following a whole foods, Paleo diet, and eliminating processed foods, excess sodium in your diet will be drastically reduced. Thus, you can be confident in following your own natural taste for salt when adding it to your food during preparation. In other words, there are few reasons to deprive yourself of salt!




Reader Comments
to our Newsletter