
© Gregor Schuster/GettyWhere you live may affect the allergies you are prone to.
We were just settling down for our flight when the captain's voice came over the PA system. "Ladies and gentlemen, I am sorry to disturb you, but we have a passenger on board who has a severe nut allergy. Could I ask you please not to open or eat any food that contains nuts for the duration of the flight? I am sorry for any inconvenience. We hope you enjoy your flight."
It was no coincidence that at the time I was on my way to a conference on food allergy in Vienna, Austria. Hazel Gowland, food adviser to the The Anaphylaxis Campaign in the UK, was travelling for the same reason, and it was for her benefit that the captain made his request.
While such an announcement may not be an everyday occurrence, most of us are familiar with the idea that peanuts can trigger a life-threatening allergic reaction. But peanuts aren't the biggest concern in every country. Passengers from Greece, where peanut allergy is rather rare, might have been more concerned about the melon in the fruit salad. A passenger from the south of Italy might have pushed the in-flight apple juice to one side for fear that it might trigger a skin rash and stomach pains, a reaction that would puzzle a compatriot from northern Italy.
Why such regional differences exist is just one of the many mysteries surrounding food allergies. Why, for example, do some migrants from east Asia develop an allergy to jackfruit when they move to northern Europe? Then there's the question of what constitutes an allergic reaction in the first place, whether there's ever a "safe" level of an allergen, and what should be done to label foods to warn people that an allergen may be present.
The Vienna conference, which took place in May this year, is part of an effort to get to the bottom of some of these mysteries. An international task force dubbed EuroPrevall, headed by biochemist Clare Mills at the Institute of Food Research in Norwich, UK, is measuring the prevalence and variation in food allergies across Europe and also in Ghana, Australia, India and China. The results are now rolling in, highlighting some of the regional anomalies and even shedding light on the basis of some of the food allergies.
One obstacle in interpreting previous research has been that different teams used different methods to test for food allergies, and much of the available data comes from subjects self-reporting their allergies without any medical tests. In 2007, a meta-analysis of more than 900 studies, led by toxicologist Charlotte Madsen of the Technical University of Denmark in Søborg and Roberto Rona, an epidemiologist at King's College London, concluded that proven food allergy affects somewhere between 1 person in 100, and 1 in 20. For the self-reported surveys, results varied even more widely, from fewer than 1 in 30 to more than 1 in 3 (
The Journal of Allergy and Clinical Immunology, vol 120, p 638). That variation may have been due in part to differences between the methods used by different studies, but as studies were conducted in many different situations across Europe it could also have due to regional differences in the prevalence of food allergies.
The EuroPrevall researchers set out to study the regional differences more closely. If links could be found between the prevalence of particular allergies and local eating habits and environmental conditions, this might shed light on what gives rise to some food allergies in the first place.
At the Vienna meeting, researchers discussed the patterns emerging from their research. For adults and children over 3 years old, hazelnuts and apples turn out to be the most common triggers of food allergies in Europeans reporting to clinics - not peanut allergy, as many people might expect. These reports from clinics have also thrown up a surprising new player: sunflower-seed allergy. Although something of a rarity, it may become more common as sunflower seeds are increasingly appearing in food. To make matters worse, the allergen involved seems to be particularly potent. "The proportion of severe reactions is higher than for peanut," says Montserrat Fernández Rivas, an allergologist from the San Carlos Clinical Hospital in Madrid, Spain.
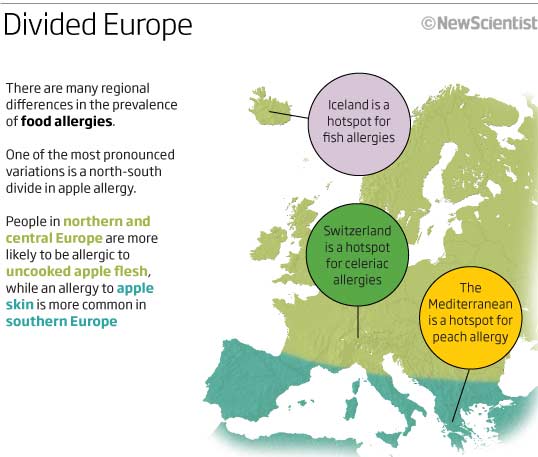
Perhaps most striking are the regional differences. "Peach and melon allergy is particularly common in the Mediterranean - in Spain and Greece," says Fernández Rivas. Reports from clinics suggest that Iceland is a hotspot for fish allergy and Switzerland has a higher rate of celeriac allergy than elsewhere.
These regional variations are likely to be due in part to differences in eating habits, causing people to be exposed to different allergens. But that alone cannot explain a pronounced north-south divide in the type of apple allergy people experience. In northern Europe, people react to the uncooked flesh of apples, whereas in the south it's the skin that sets them off, whether it's cooked or not. What could be the cause of this strange invisible dividing line that skims across south-west France, cuts through Italy close to Florence, and continues eastwards through the middle of the Black Sea?
Significantly, this line marks the southern limit of the birch tree, a plant whose pollen is one of the causes of hay fever in northern Europe. Clues for this link lie in the different proteins found in various parts of the fruit: the flesh harbours an allergenic protein called Mal d 1, while the skin is relatively rich in Mal d 3. The structure and composition of the Mal d 1 protein strongly resembles the allergenic protein Bet v 1 found in birch pollen. This means that people who suffer from birch pollen allergy may be primed to overreact to Mal d 1 - explaining the prevalence of the allergy to apple flesh in this region.
© New Scientist
A similar cross-reaction explains the allergy to apple skin found in southern Europe. In this case, a prior sensitisation to the Pru p 3 protein in peaches, which bears a strong similarity to Mal d 3, seems to be the culprit. What's more, Mal d 1 breaks down when heated while Mal d 3 is heat resistant, which neatly explains why northern Europeans are fine with cooked apples and pasteurised apple juice but apple-allergic people in the south cannot cope with these fruit in any form (see map).
Other reported cross-reactions include a link between house-dust-mite faeces and shrimp allergy, and another between mugwort pollen and an allergy to carrots, celery and sunflower seeds. There are likely to be many others, since many allergens seem to share similarities in their amino acid sequences that might confuse the immune system.
In fact, between 2005 and 2008 Mills and Heimo Breiteneder, a molecular allergist at the Medical University of Vienna, and their colleagues completed a series of studies showing the majority of allergens originating in fruit and vegetables belong to just four of the 10,000 or so recognised families of proteins, and most of the animal-food allergens to just three families (
The Journal of Allergy and Clinical Immunology, vol 115, p 163 and vol 121, p 847). Bet v 1, for example, causes cross-reactions with several other members of its protein family, and as a result people who have birch pollen allergy stand a good chance of being allergic to apple, celery, plums and several other common foods.
This also explains why some migrants from east Asia to northern Europe suddenly develop an allergic reaction to jackfruit once they have come into contact with birch pollen. The allergen in jackfruit does not on its own sensitize the immune system, but once birch pollen has done the job, the immune system may react to jackfruit too.
Lookalike allergensThese numerous examples of cross-reactions raise another question: why does Bet v 1 cause an allergy to the Mal d 1 protein but not the other way around? Researchers believe it's because Bet v 1 enters the body via the lungs, so it is not broken down by digestion and can reach the bloodstream intact, where it activates the immune system. Mal d 1, on the other hand, is broken down during digestion, so it loses its capacity to prime the immune system. Once the immune system has been stimulated by the Bet v 1, it may then become sensitive to similar looking proteins like Mal d 1 - sensitive enough to trigger a reaction when it comes into contact with the mouth.
Cross-reactions are not the end of the story, however. Other environmental factors probably play a role: for instance, cigarette smoking has recently been shown to aggravate allergies. Genetics are also thought to be important.
If the pattern of the various allergies across the world is a confusing story, the practices and regulations designed to protect vulnerable people from potentially fatal allergic reactions are no clearer. Even the apparently sensible precaution of printing warnings on food labels is fraught with complications.
A study in 2005 by allergy researcher Steve Taylor of the University of Nebraska in Lincoln showed that of the 200 food products that he examined labelled "May contain nuts", only 10 per cent actually did, and many of those contained only minute amounts (
Journal of Allergy and Clinical Immunology, vol 120, p 171). Nor does the absence of a warning label guarantee that the food is safe for people who are allergic. In Europe, for example, an examination of various types of chocolate showed that half of those without a warning contained hazelnut (
Food Additives and Contaminants, vol 24, p 1334).
Part of the problem with labelling goes back to the practicalities of industrial production. Since the same machinery may be used to make many different products, it is often difficult to guarantee that the foods will not become cross-contaminated. As a result companies play it safe and put warning labels on products that may not in fact contain high enough levels of allergen to have any effect. This raises the danger that people will start ignoring the message, putting themselves at risk of consuming food that does contain a dangerous level of the allergen. "The 'may contain' labelling is becoming so devalued," says Sue Hattersley of the UK's Food Standards Agency.
So what should companies be doing to inform consumers? Individuals are so diverse that it's hard to define a level that guarantees no one will have an adverse reaction, so instead they must just try to minimise the risk. "What level of risk can be considered tolerable?" asks René Crevel, a toxicologist at food manufacturer Unilever's labs in Colworth, UK. The threshold level at which some kind of reaction can occur may be less than a thousandth of a potentially fatal dose, so where do you draw the line?
There is progress, at least for people who are allergic to gluten in wheat. A new European guideline, which comes into force in 2012, means that foods containing less than 20 parts per million of gluten can be labelled 'gluten free'. And many allergists reckon there is now enough data to start giving serious thought to a specific limit below which foods can be deemed free of peanut allergens.
Even if the food industry does find a better way to label foods, there will always be the danger of an accidental exposure to high concentrations of an allergen. "The main risk is from caterers and restaurants," says Frans Timmermans of the Netherlands Anaphylaxis Network. "In the UK most deaths are from curries, weddings, parties, and not knowing what satay and pesto are," says Gowland, my fellow passenger on the Vienna flight. "Otherwise, it's often down to not knowing in the first place that they were allergic."
Some people with a severe food allergy are afraid of even a passing exposure to an allergen, and this has led some to ask for bans of potentially dangerous foods in public areas such as schools, to reduce the risk. Some American high schools, for example, are now banning food products containing peanuts. In one instance, a school bus was evacuated and then taken out of service to be decontaminated after a single peanut escaped from its wrapper. "People in favour of various bans feel it is just easier to have the food eliminated," says Scott Sicherer, an allergist at the Mount Sinai School of Medicine in New York City.
Others believe that such measures are out of proportion to the real danger. Writing in the medical journal
BMJ last year, medical sociologist Nicholas Christakis of Harvard Medical School in Boston observed that efforts by US schools to prevent students being exposed to peanuts "represent a gross overreaction to the magnitude of the threat" (
BMJ, vol 337, p 1384). According to Timmermans, parents can sometimes become so worried about the possible threat to their children that they cause the children themselves psychological distress.
But what of my flight: was the captain right to ask that no nut products be consumed on the plane? Timmermans says he is surprised by the request. His daughter, who is also highly allergic to peanuts, would be able to sit next to someone eating a peanut dish without experiencing a reaction, he says, though he admits it would make her uneasy.
Others are more sympathetic. "I have no problem with pilots making this announcement," says Taylor. "Nut-allergic passengers can be at risk of rather scary and uncomfortable reactions from the food of others." It may seem extreme and inconvenient to fellow passengers but, for Gowland and her fellow sufferers, the risk is too real to ignore.
Reader Comments
to our Newsletter