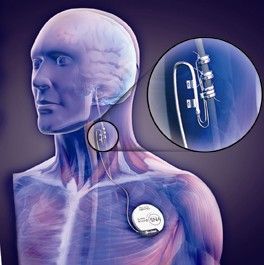
Vagus Nerve Stimulator
Thanks to an exchange of e-mails on a list that includes journalists Jeanne Lenzer and Shannon Brownlee (whose great work I've previously blogged about), I was directed to an article (subscription required) that I failed to make note of when it came out nearly two years ago. It provides useful background to an issue that has become even more heated this last year, the medical device safety oversight problem (see for example
here).
Lenzer and Brownlee looked in depth at the vagus nerve stimulator manufactured by Cyberonics, a device in which a pacemaker-type pack is surgically inserted near the collarbone, and electrodes are wrapped around the vagus nerve in the neck. The device was intended at first for a select population of patients with a particular type of epilepsy that's resistant to all drug treatment. Like many devices and drugs (and in keeping with the
Inverse Benefit Law), once having gotten the camel's nose into the tent, Cyberonics is now claiming that the stimulator can be used for a large number of other conditions, notably depression, and perhaps obesity and traumatic brain injury (stay tuned for hair loss and bad breath). All such uses rely on the purported safety of the device, which is what Lenzer and Brownlee zeroed in on.
In 1997, Cyberonics went to the FDA to get initial approval of the stimulator for epilepsy. They presented three studies to document the device's effectiveness and safety. One review panelist noted that 17 of the 1000 subjects who'd had the device implanted had died, and asked what was up with that. The explanation offered by the company and other panelists is that people who have that sort of hard-to-treat epilepsy have a high death rate because periodically those seizures cause cardiac and respiratory arrest. So deaths were due to the disease and not the device.
The FDA bought this explanation but added a caveat--Cyberonics got approval conditionally upon conducting a post-marketing surveillance study to address the concern about possible excess deaths.This, as Lenzer and Browlnee explain, is not an unusual measure--the studies needed to lead to drug or device approval are often, of necessity, too small to detect rare but serious adverse effects, and only after a drug or device is more widely used may such effects become apparent.
But here's where the story gets interesting. Lenzer and Brownlee then went after the data accumulated by the company during this mandated post-marketing study phase. They found several very worrisome things. First,
there were at least isolated reports of deaths or near-misses that seemed quite clearly to be due to the device. (One patient who survived was observed to have his heart stop at exactly the intervals at which the stimulator fired, and the heart stoppages ceased with the device was turned off.) When asked how many of these events had occurred, or how often, Cyberonics said they didn't know, because mortality statistics were not one of the planned endpoints in any of its trials. And despite the fact that the FDA had ordered these studies because of concerns about mortality, no one at the FDA seemed the least bit worried about the fact that Cyberonics had set up its studies deliberately to exclude mortality data.
For many years, British sociologist John Abraham has written about regulatory capture--what happens when a government agency that is supposed to regulate an industry ends up becoming so closely tied to industry that it becomes a tool rather than a watchdog. When the Institute of Medicine
weighed in on how inadequate the current regulations are for monitoring device safety, one might have thought that the FDA would appreciate the help they were getting to call for more stringent regulations--but instead the FDA went out of its way to defend the current inadequate practices and to blast the IOM's conclusions. Since then, as per previous blog posts referred to above, the device industry has unleashed a lobbying armageddon on Congress, demanding less rather than more regulation of device safety lest a single good job in the US be sent overseas.
The combination of merciless lobbying plus FDA capture makes it highly unlikely that we'll see a day anytime soon when the US public can have much confidence that medical devices are adequately checked for safety. How it works out that there's a huge media outcry if a single person dies from E.coli in their lettuce, but dozens or hundreds can die due to malfunctioning medical devices without anyone losing any sleep, needs to be better explained.
ReferenceLenzer J, Brownlee S. Why the FDA can't protect the public.
BMJ 341:966-68, 6 November 2010.
Due to the limited space allowed for comments, I have posted mine at my site. Please be kind enough to read it, There is so much more to Cyberonic$. They are a menace and danger to society. They feed on the hardships of the most vulnerable. They have caused 1000's of deaths and 10,000's of ruined lives. Now they are swaying the military to use those coming back from war.
[Link]