Since the 1930s, doctors have been jolting the brains of depressed patients with electricity to relieve their symptoms. The treatment, known as electroconvulsive therapy (ECT), works, but it can cause memory loss and confusion and lead to difficulty forming new memories. Today, physicians generally limit it to patients who are severely ill, including those at risk for suicide. Now, a brain-imaging study highlights the part of the brain most affected, perhaps pointing to safer, less-invasive ways to achieve the same results.
Depression may be caused by an overactive brain, says physicist and neuroscientist Christian Schwarzbauer of the University of Aberdeen in the United Kingdom. "There may be so much internal communication that the brain becomes preoccupied with itself, less able to process information coming in from the outside world," he says, noting that studies have found that people with depression have heightened connectivity among brain networks involved in paying attention, monitoring internal and external cues, remembering the past, and controlling emotions.
In a 2010 study, psychiatrist Yvette Sheline and colleagues at Washington University School of Medicine in St. Louis, Missouri, found that these overactive networks converged on a common point in a region called the dorsal medial prefrontal cortex. This common point, dubbed the dorsal nexus, may "hot wire" the brain networks together in a way that leads to depression, the authors hypothesized.
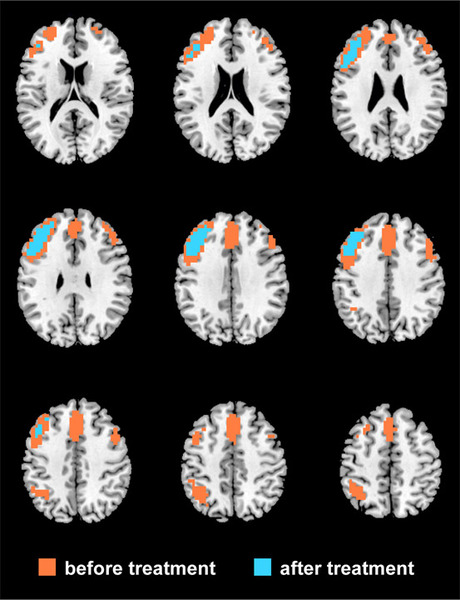
It may be this nexus that's affected by ECT, according to the new findings. In a study led by psychiatrist Ian Reid of Aberdeen, Schwarzbauer and colleagues performed functional magnetic resonance imaging (fMRI) scans of nine depressed patients before and after ECT. Rather than focusing on activity in previously suspected brain areas, the researchers examined connectivity in the brain as a whole, examining changes in blood oxygenation in about 27,000 points known as voxels (the 3D imaging equivalent of pixels on a computer screen). Voxels were considered to be highly connected if their changes in blood oxygenation were strongly correlated - if one went up and the other went up to a similar degree.
After treatment with ECT, connectivity was dramatically decreased in one cluster of voxels around an area called the dorsolateral prefrontal cortex, the researchers report today in the Proceedings of the National Academy of Sciences. Decreases in connectivity reflected improvements in symptoms, as reported by the patients. The area of decreased connectivity includes the dorsal nexus previously identified by Sheline and colleagues. This finding indicates that ECT reduces the influence of the dorsolateral prefrontal cortex on this nexus.
Because the dorsal nexus is a place where attention, memory, and emotion all converge, its emergence as the target of ECT explains both the therapy's success and the side effects of memory impairment, the authors write.
"This is an important study. It provides insight into a likely mechanism for ECT," Sheline says. She adds that both antidepressant treatment and cognitive therapy have been shown to reduce excessive connectivity in some areas.
But research psychologist Jennifer Perrin, co-author of the new paper, cautions: "It still isn't known whether these approaches reduce connectivity in the specific area that we found." She says further research is needed to see whether this effect is unique to ECT or is a feature of other treatments as well.
Perrin says the finding may open the door to treatments that target the area more directly. For example, in transcranial magnetic stimulation, a magnetic field is passed over the scalp above this part of the brain; a similar study could explore whether this technique could be made more effective. The authors' method of analyzing connectivity could also be used to study other disorders, such as schizophrenia, autism, or dementia, she says.



You'll never convince me of that!
It's a barbaric practice that's kind of like slapping a person really hard to get them to wake up.
ECT is a lie. If it works, show me the people who it "worked" on, now perfectly cheerful and leading full and productive lives.
This planet is full of trauma-based "solutions" to the problems people face. They are a part of a long and tragic con game, and nothing more.
If you really want to a person to cheer up, try tickling them. The point is, misemotion is caused by too much attention on misemotional incidents. Coax a person to devote more attention to present time, and they will generally begin to react more appropriately.
Too bad that present time, for a lot of us, is no great shakes, either.